A nurse is caring for a newborn whose mother was taking methadone during her pregnancy.
Which of the following findings indicates the newborn is experiencing withdrawal?
Acrocyanosis
Bradycardia
Bulging fontanels
Hypertonicity
The Correct Answer is D
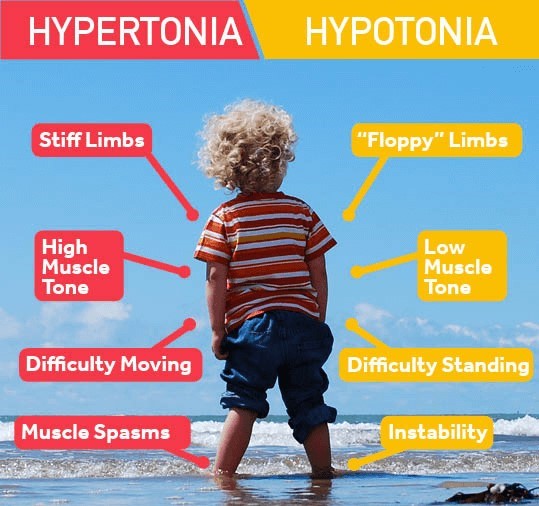
Hypertonicity is a sign of increased muscle tone and stiffness, which can indicate that the newborn is experiencing withdrawal from methadone exposure in utero. Methadone is an opioid medication that can cross the placenta and cause neonatal abstinence syndrome (NAS) in the newborn.
Choice A, acrocyanosis, is wrong because it is a normal finding in newborns.
Acrocyanosis is a bluish discoloration of the hands and feet due to immature peripheral circulation. It usually resolves within the first 24 to 48 hours of life.
Choice B, bradycardia, is wrong because it is not a typical sign of withdrawal.
Bradycardia is a slow heart rate, usually less than 100 beats per minute in newborns. It can be caused by hypoxia, hypothermia, hypoglycemia, or vagal stimulation.
Choice C, bulging fontanels, is wrong because it is a sign of increased intracranial pressure, not withdrawal. Bulging fontanels can be caused by meningitis, hydrocephalus, or hemorrhage.
Normal ranges for newborn vital signs are as follows:
- Heart rate: 120 to 160 beats per minute
- Respiratory rate: 30 to 60 breaths per minute
- Temperature: 36.5 to 37.5°C (97.7 to 99.5°F)
- Blood pressure: 60 to 80 mm Hg systolic and 40 to 50 mm Hg diastolic
Nursing Test Bank
Naxlex Comprehensive Predictor Exams
Related Questions
Correct Answer is A
Explanation
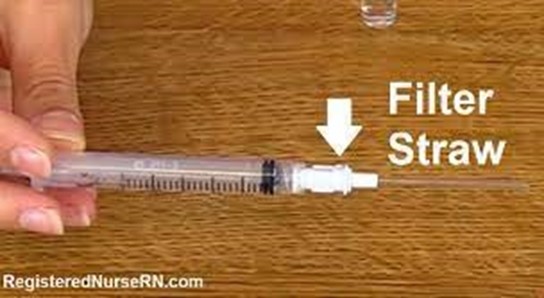
This is because glass ampules can leave small shards of glass in the solution, which can be harmful if injected into the client. A filter needle has a small mesh that traps any glass particles and prevents them from entering the syringe.
Choice B is wrong because the nurse should break the neck of the ampule away from their body to avoid injury from the glass.
Choice C is wrong because the nurse should use a different needle to inject the client after withdrawing the medication with a filter needle. This is to prevent contamination and reduce pain for the client.
Choice D is wrong because the nurse should dispose of the ampule in a sharps container, not in the trash can. This is to prevent injury and infection from the broken glass.
Correct Answer is D
Explanation
The correct answer is choice D. The client is oriented times three.
This means that the client knows who they are, where they are, and what time it is. This indicates a high level of consciousness and a normal Glasgow coma scale (GCS) rating of 15.
Choice A is wrong because the client withdraws from pain.
This means that the client reacts to a painful stimulus by pulling away from it. This indicates a lower level of consciousness and a GCS rating of 4 for motor response.
Choice B is wrong because the client is unable to obey commands.
This means that the client does not follow simple instructions such as moving a limb or opening their eyes. This indicates a lower level of consciousness and a GCS rating of 1 or 2 for motor response.
Choice C is wrong because the client opens eyes to sound.
This means that the client does not open their eyes spontaneously, but only when they hear a loud noise. This indicates a lower level of consciousness and a GCS rating of 3 for eye opening.
The Glasgow coma scale is a clinical tool used to assess the level of consciousness of a person after a brain injury.
It consists of three tests: eye opening, verbal response, and motor response.
Each test has a score range from 1 to 6, with higher scores indicating higher levels of consciousness. The total score ranges from 3 to 15, with lower scores indicating higher risk of death.
Whether you are a student looking to ace your exams or a practicing nurse seeking to enhance your expertise , our nursing education contents will empower you with the confidence and competence to make a difference in the lives of patients and become a respected leader in the healthcare field.
Visit Naxlex, invest in your future and unlock endless possibilities with our unparalleled nursing education contents today
Report Wrong Answer on the Current Question
Do you disagree with the answer? If yes, what is your expected answer? Explain.
Kindly be descriptive with the issue you are facing.
