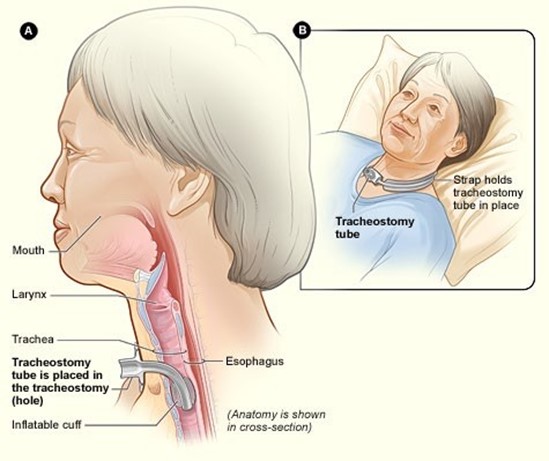
A nurse is caring for a client with a tracheostomy. The client's partner has been taught to perform suctioning. Which of the following actions by the partner should indicate to the nurse a readiness for the client's discharge?
Performing the procedure independently
Attending a class given about tracheostomy care
Verbalizing all steps in the procedure
Asking appropriate questions about suctioning
The Correct Answer is A
Performing the procedure independently is the best indicator of the partner's readiness for the client's discharge, as it demonstrates competence and confidence in suctioning. Suctioning is a skill that requires practice and supervision until mastery is achieved. The nurse should observe and evaluate the partner's performance of suctioning and provide feedback and reinforcement as needed.
b) Attending a class given about tracheostomy care is a good action by the partner, but not the best indicator of readiness for the client's discharge. Attending a class can provide information and education about tracheostomy care, but it does not necessarily translate into skill acquisition or application. The nurse should assess the partner's understanding and retention of the information and provide additional teaching or clarification as needed.
c) Verbalizing all steps in the procedure is a good action by the partner, but not the best indicator of readiness for the client's discharge. Verbalizing all steps in the procedure can help the partner remember and follow the correct sequence and technique of suctioning, but it does not necessarily reflect actual performance or ability. The nurse should observe and verify that the partner is doing what they are saying and correct any errors or omissions as needed.
d) Asking appropriate questions about suctioning is a good action by the partner, but not the best indicator of readiness for the client's discharge. Asking appropriate questions about suctioning can show interest and involvement in learning and caring for the client, but it does not necessarily indicate competence or confidence in suctioning. The nurse should answer the partner's questions and provide additional resources or referrals as needed.
Nursing Test Bank
Naxlex Comprehensive Predictor Exams
Related Questions
Correct Answer is B
Explanation
A humidifier bottle adds moisture to the oxygen, which prevents drying and irritation of the nasal mucosa
and enhances gas exchange.
a. Remove the nasal cannula while the client eats. This is not advisable, as the client may become hypoxic during eating, especially if they have pneumonia and impaired lung function. The nurse should monitor the client's oxygen saturation and respiratory status during meals and adjust the oxygen delivery device as needed.
c. Secure the oxygen tubing to the bed sheet near the client's head. This is not safe, as it can cause entanglement, dislodgement, or kinking of the tubing, which can compromise oxygen delivery and cause injury to the client.
d. Apply petroleum jelly to the nares as needed to soothe mucous membranes. This is not recommended, as petroleum products can ignite in the presence of oxygen and cause burns or fire. A water-based lubricant should be used instead.

Correct Answer is B
Explanation
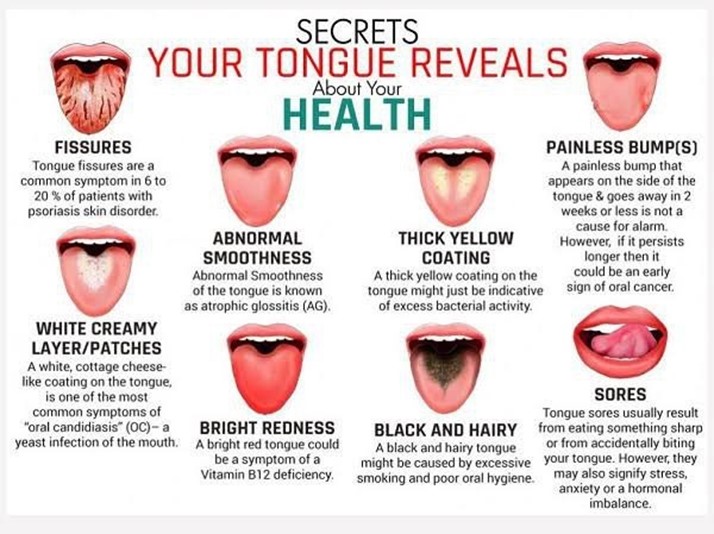
White coating in the mouth, also known as oral candidiasis or thrush, is a serious adverse effect of fluticasone/salmeterol, which is a combination of an inhaled corticosteroid and a long-acting beta2 agonist. It is caused by fungal infection of the oral cavity due to suppression of the normal flora by the corticosteroid component. The client should report this symptom to the provider, as it may require antifungal treatment and discontinuation of the medication.
a) Dry oral mucous membranes is a common and mild adverse effect of fluticasone/salmeterol, which can be relieved by drinking water, chewing sugarless gum, or using artificial saliva. It does not require reporting to the provider or stopping the medication.
c) Sedation is not an adverse effect of fluticasone/salmeterol, but it may be caused by other medications, such as antihistamines, opioids, or benzodiazepines. The client should avoid driving or operating machinery if sedated and consult with the provider about possible drug interactions.
d) Increased appetite is not an adverse effect of fluticasone/salmeterol, but it may be caused by other factors, such as stress, boredom, or hormonal changes. The client should maintain a balanced diet and exercise regularly to prevent weight gain and promote health.
Whether you are a student looking to ace your exams or a practicing nurse seeking to enhance your expertise , our nursing education contents will empower you with the confidence and competence to make a difference in the lives of patients and become a respected leader in the healthcare field.
Visit Naxlex, invest in your future and unlock endless possibilities with our unparalleled nursing education contents today
Report Wrong Answer on the Current Question
Do you disagree with the answer? If yes, what is your expected answer? Explain.
Kindly be descriptive with the issue you are facing.
