A nurse is caring for a client who is in active labor and reports sudden, severe lower abdominal pain. The nurse observes a drop in the client's blood pressure and notes cool skin and pallor. The fetal heart rate tracing shows prolonged bradycardia. Which of the following complications should the nurse suspect?
Amniotic fluid embolism
Umbilical cord prolapse
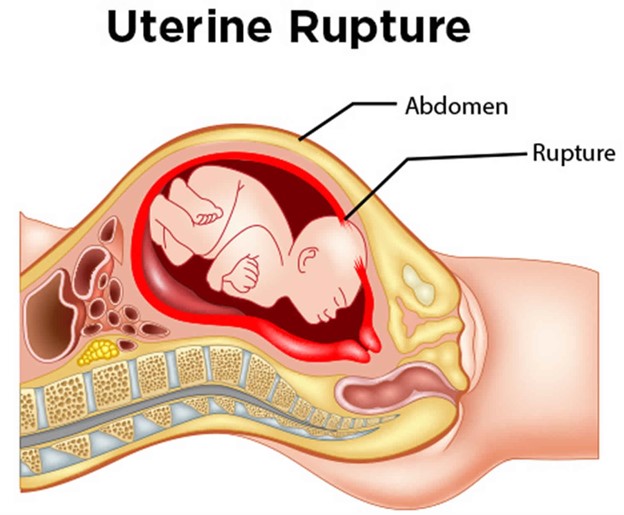
Uterine rupture
Placenta previa
The Correct Answer is C
Uterine rupture. The sudden, severe lower abdominal pain, drop in blood pressure, and signs of shock such as cool skin and pallor all point to a potential intra-abdominal hemorrhage most likely due to Uterine rupture. Additionally, the prolonged bradycardia on the fetal heart rate tracing indicates that the baby may be experiencing fetal distress due to a compromised blood supply. Amniotic fluid embolism triggers an allergic reaction, causing a sudden onset of respiratory distress, hypotension, and cardiac arrest. Option D, placenta previa, occurs when the placenta implants in the lower uterine segment, partially or completely covering the cervical os. This can lead to painless vaginal bleeding but typically does not present with sudden, severe abdominal pain or signs of shock.
Nursing Test Bank
Naxlex Comprehensive Predictor Exams
Related Questions
Correct Answer is {"dropdown-group-1":"C","dropdown-group-2":"A"}
Explanation
The correct answer is Eating a well-balanced diet and exercising for 30 minutes per day.
Itcan help to reduce stress and improve mood, which can help to prevent postpartum depression. This provide the body with the essential nutrients it needs to function properly and maintain good health. Exercise can help to reduce stress and improve mood by releasing endorphins, which are hormones that can help to improve mood and reduce stress.
Correct Answer is A
Explanation
The correct answer is choice A: Fortified soy milk. Vitamin B12 is found in animal products, so vegans are at risk of vitamin B12 deficiency. Fortified soy milk is a good source of vitamin B12 for vegans.
Choice B, brown rice, choice C, fresh citrus fruits, and choice D, raw carrots, are not good sources of vitamin B12.
Whether you are a student looking to ace your exams or a practicing nurse seeking to enhance your expertise , our nursing education contents will empower you with the confidence and competence to make a difference in the lives of patients and become a respected leader in the healthcare field.
Visit Naxlex, invest in your future and unlock endless possibilities with our unparalleled nursing education contents today
Report Wrong Answer on the Current Question
Do you disagree with the answer? If yes, what is your expected answer? Explain.
Kindly be descriptive with the issue you are facing.
