A nurse is caring for a client who has emphysema. Which of the following findings should the nurse expect to assess in this client? (Select all that apply.)
Dyspnea
Barrel chest
Deep respirations
Clubbing of the fingers
Bradycardia
Correct Answer : A,B,D
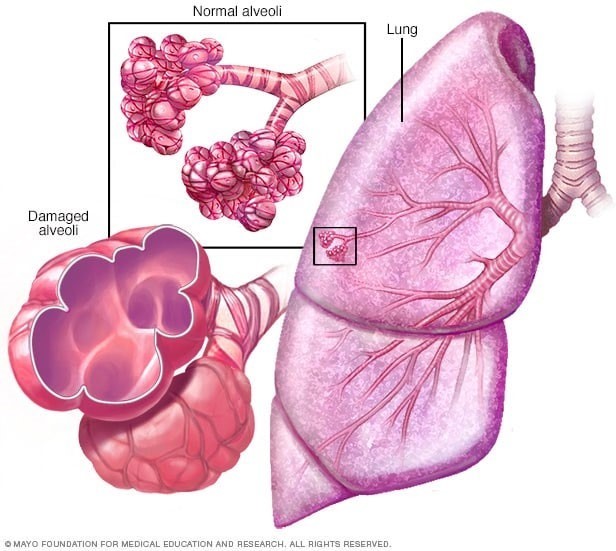
These findings are expected to be assessed in a client who has emphysema, which is a type of chronic obstructive pulmonary disease (COPD) characterized by destruction and enlargement of alveoli, loss of elastic recoil, and air trapping. These changes impair gas exchange and oxygenation, leading to chronic hypoxia and hypercapnia.
a) Dyspnea, or difficulty breathing, is a common symptom of emphysema, as the client has reduced lung capacity and increased work of breathing. Dyspnea may be worse with exertion, stress, or infection, and may cause anxiety and fatigue. The nurse should monitor the client's respiratory rate, rhythm, depth, and effort, and provide oxygen therapy as prescribed.
b) Barrel chest, or increased anteroposterior diameter of the chest, is a physical sign of emphysema, as the client has chronic air trapping and hyperinflation of the lungs. Barrel chest may also cause kyphosis, or curvature of the spine, and reduced chest wall movement. The nurse should measure the client's chest circumference and observe for any deformities or asymmetry.
d) Clubbing of the fingers, or enlargement and rounding of the nail beds, is a late sign of emphysema, as the client has chronic hypoxia and tissue ischemia. Clubbing may also affect the toes and ears, and may indicate pulmonary or cardiac disease. The nurse should inspect the client's nails for shape, color, angle, and capillary refill.
c) Deep respirations are not expected to be assessed in a client who has emphysema, as the client has shallow and rapid breathing due to air trapping and reduced lung compliance. Deep respirations may indicate other conditions, such as metabolic acidosis or anxiety. The nurse should assess the client's arterial blood gas levels and provide reassurance and relaxation techniques as needed.
e) Bradycardia, or slow heart rate, is not expected to be assessed in a client who has emphysema, as the client has tachycardia or normal heart rate due to hypoxia and increased sympathetic stimulation. Bradycardia may indicate other conditions, such as medication side effects, vagal stimulation, or heart block. The nurse should monitor the client's pulse rate, rhythm, quality, and electrocardiogram as indicated.
Nursing Test Bank
Naxlex Comprehensive Predictor Exams
Related Questions
Correct Answer is A
Explanation
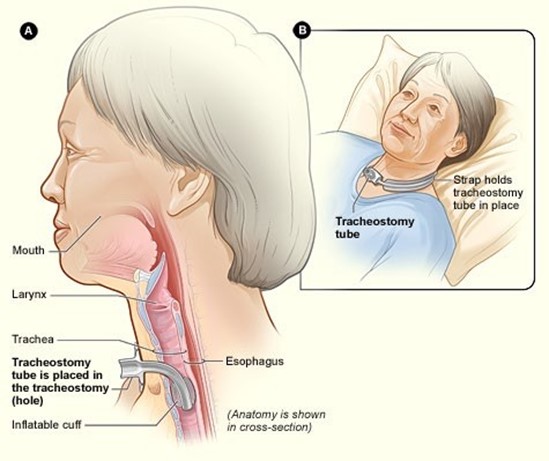
Performing the procedure independently is the best indicator of the partner's readiness for the client's discharge, as it demonstrates competence and confidence in suctioning. Suctioning is a skill that requires practice and supervision until mastery is achieved. The nurse should observe and evaluate the partner's performance of suctioning and provide feedback and reinforcement as needed.
b) Attending a class given about tracheostomy care is a good action by the partner, but not the best indicator of readiness for the client's discharge. Attending a class can provide information and education about tracheostomy care, but it does not necessarily translate into skill acquisition or application. The nurse should assess the partner's understanding and retention of the information and provide additional teaching or clarification as needed.
c) Verbalizing all steps in the procedure is a good action by the partner, but not the best indicator of readiness for the client's discharge. Verbalizing all steps in the procedure can help the partner remember and follow the correct sequence and technique of suctioning, but it does not necessarily reflect actual performance or ability. The nurse should observe and verify that the partner is doing what they are saying and correct any errors or omissions as needed.
d) Asking appropriate questions about suctioning is a good action by the partner, but not the best indicator of readiness for the client's discharge. Asking appropriate questions about suctioning can show interest and involvement in learning and caring for the client, but it does not necessarily indicate competence or confidence in suctioning. The nurse should answer the partner's questions and provide additional resources or referrals as needed.
Correct Answer is ["A","C","E"]
Explanation
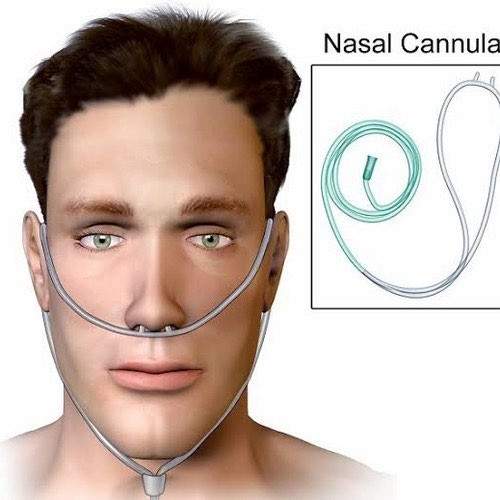
These are important safety and comfort measures for a client who uses home oxygen therapy via a nasal cannula.
The other options are not correct because:
b. Verify the oxygen flow rate every other day. This is not frequent enough, as the flow rate should be checked at least daily and whenever the client feels short of breath or has changes in vital signs.
d. Apply petroleum ointment to nares if they become dry and irritated. This is not recommended, as petroleum products can ignite in the presence of oxygen and cause burns or fire. A water-based lubricant should be used instead.
Whether you are a student looking to ace your exams or a practicing nurse seeking to enhance your expertise , our nursing education contents will empower you with the confidence and competence to make a difference in the lives of patients and become a respected leader in the healthcare field.
Visit Naxlex, invest in your future and unlock endless possibilities with our unparalleled nursing education contents today
Report Wrong Answer on the Current Question
Do you disagree with the answer? If yes, what is your expected answer? Explain.
Kindly be descriptive with the issue you are facing.
