A nurse is assessing a client who has postoperative atelectasis and is hypoxic. Which of the following manifestations should the nurse expect?
Lethargy
Bradycardia
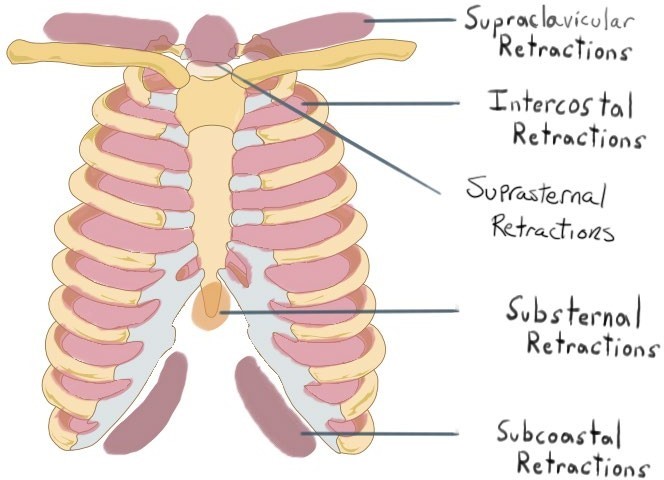
Intercostal retractions
Bradypnea
The Correct Answer is C
Intercostal retractions, or the inward movement of the chest wall between the ribs, are a sign of respiratory distress and hypoxia. They indicate increased work of breathing and reduced lung expansion, which are common in clients who have postoperative atelectasis. Atelectasis is a collapse of alveoli in a part of the lung, which impairs gas exchange and oxygenation.
a) Lethargy, or a state of reduced mental alertness and energy, is not a typical manifestation of hypoxia. It can be caused by other factors, such as pain, medication, infection, or electrolyte imbalance. Hypoxia usually causes restlessness, anxiety, or confusion.
b) Bradycardia, or a slow heart rate, is not a typical manifestation of hypoxia. It can be caused by other factors, such as medication, vagal stimulation, or heart block. Hypoxia usually causes tachycardia, or a fast heart rate, as the body tries to compensate for the low oxygen level.
d) Bradypnea, or a slow respiratory rate, is not a typical manifestation of hypoxia. It can be caused by other factors, such as medication, brain injury, or metabolic alkalosis. Hypoxia usually causes tachypnea, or a fast respiratory rate, as the body tries to increase oxygen intake and carbon dioxide elimination.
Nursing Test Bank
Naxlex Comprehensive Predictor Exams
Related Questions
Correct Answer is B
Explanation
A humidifier bottle adds moisture to the oxygen, which prevents drying and irritation of the nasal mucosa
and enhances gas exchange.
a. Remove the nasal cannula while the client eats. This is not advisable, as the client may become hypoxic during eating, especially if they have pneumonia and impaired lung function. The nurse should monitor the client's oxygen saturation and respiratory status during meals and adjust the oxygen delivery device as needed.
c. Secure the oxygen tubing to the bed sheet near the client's head. This is not safe, as it can cause entanglement, dislodgement, or kinking of the tubing, which can compromise oxygen delivery and cause injury to the client.
d. Apply petroleum jelly to the nares as needed to soothe mucous membranes. This is not recommended, as petroleum products can ignite in the presence of oxygen and cause burns or fire. A water-based lubricant should be used instead.

Correct Answer is C
Explanation
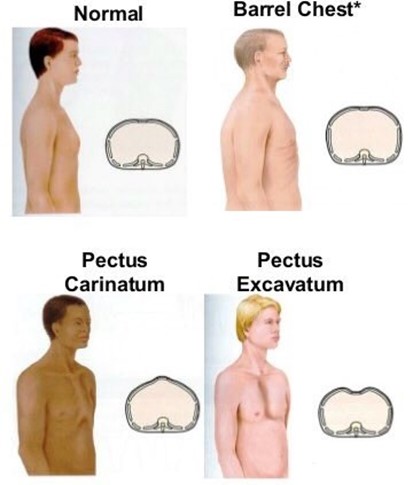
Increased anteroposterior diameter of the chest, also known as barrel chest, is a common finding in clients who have COPD with emphysema. It is caused by chronic air trapping and hyperinflation of the lungs, which results in fattening of the diaphragm and widening of the rib cage.
a) Oxygen saturation level 96% is within the normal range of 95% to 100% and does not indicate hypoxemia or impaired gas exchange. Clients who have COPD with emphysema typically have lower oxygen saturation levels, ranging from 88% to 92%.
b) Respiratory alkalosis is a condition in which the blood pH is elevated due to decreased carbon dioxide levels. It is caused by hyperventilation, which can occur in response to hypoxia, anxiety, or pain. Clients who have COPD with emphysema usually have respiratory acidosis, which is a condition in which the blood pH is lowered due to increased carbon dioxide levels. It is caused by hypoventilation, which results from impaired lung function and airway obstruction.
d) Petechiae on chest are small red or purple spots on the skin caused by bleeding from capillaries. They are not a typical finding in clients who have COPD with emphysema, unless they have severe coughing episodes or coagulation disorders. They can indicate infection, inflammation, trauma, or vascular disease.
Whether you are a student looking to ace your exams or a practicing nurse seeking to enhance your expertise , our nursing education contents will empower you with the confidence and competence to make a difference in the lives of patients and become a respected leader in the healthcare field.
Visit Naxlex, invest in your future and unlock endless possibilities with our unparalleled nursing education contents today
Report Wrong Answer on the Current Question
Do you disagree with the answer? If yes, what is your expected answer? Explain.
Kindly be descriptive with the issue you are facing.
