A nurse is providing dietary teaching for a client who has chronic obstructive pulmonary disease. Which of the following instructions should the nurse include?
"Use a bronchodilator 1 hour before eating."
"Eat 3 large meals each day."
"Limit water intake with meals."
"Reduce protein intake."
None
None
The Correct Answer is C
A. Administration of a prescribed bronchodilator is typically recommended approximately 30 minutes prior to meals rather than 1 hour. This pharmacological timing helps reduce dyspnea and facilitates easier deglutition and mastication by improving airflow. Using it too early may result in the peak therapeutic effect tapering off before the client finishes the meal.
B. Consuming 3 large meals each day is contraindicated for clients with chronic obstructive pulmonary disease because a distended stomach can exert upward pressure on the diaphragm. This abdominal crowding significantly increases the work of breathing and leads to early satiety or respiratory distress. Clients are instead encouraged to eat 5 to 6 small, frequent, nutrient-dense meals.
C. The nurse should instruct the client to limit water or fluid intake during the actual mealtime to prevent premature gastric distention. Early fullness from fluids reduces the client’s ability to consume essential solid nutrients and calories required to support the increased metabolic demands of labored breathing. Fluids should be consumed between meals to maintain adequate hydration and thin secretions.
D. Reducing protein intake is inappropriate because these clients require high-protein and high-calorie diets to prevent muscle wasting and support the respiratory muscles. The metabolic cost of breathing in chronic obstructive pulmonary disease is significantly elevated, often leading to a state of malnutrition or cachexia. Protein is vital for tissue repair and maintaining the functional integrity of the diaphragm.
Nursing Test Bank
Naxlex Comprehensive Predictor Exams
Related Questions
Correct Answer is D
Explanation
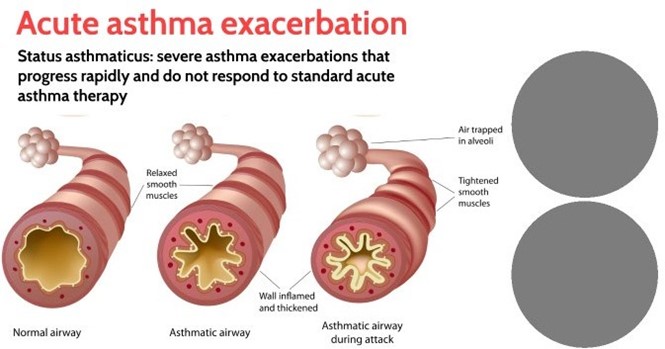
Administering a short-acting beta2-agonist (SABA), such as albuterol, is the priority intervention for the nurse to take, as it provides rapid bronchodilation and relieves bronchospasm, which are the main features of status asthmaticus. Status asthmaticus is a severe and life-threatening asthma attack that does not respond to usual treatment and requires immediate medical attention.
a) Determining the cause of the acute exacerbation is important, but not the priority intervention for the nurse to take. The cause may be an allergen, infection, stress, or exercise, but it does not affect the immediate management of status asthmaticus. The nurse should focus on restoring airway patency and oxygenation first, and then identify and avoid triggers later.
b) Obtaining a peak flow reading is important, but not the priority intervention for the nurse to take. The peak flow reading measures the maximum expiratory flow rate and indicates the degree of airway obstruction. However, it may not be feasible or accurate in a child who is experiencing status asthmaticus, as they may be too dyspneic or agitated to perform the test. The nurse should rely on other signs of respiratory distress, such as wheezes, retractions, cyanosis, or pulse oximetry.
c) Administering an inhaled glucocorticoid is important, but not the priority intervention for the nurse to take. Glucocorticoids, such as fluticasone or budesonide, reduce inflammation and mucus production in the airways, but they have a delayed onset of action and are not effective for acute asthma attacks. They are used for long-term control and prevention of asthma symptoms.
Correct Answer is A
Explanation
Answer: A
Rationale:
A) Administering a nebulized beta-adrenergic:
In the case of an acute asthma exacerbation, administering a nebulized beta-adrenergic agonist (such as albuterol) is the highest priority. These medications act quickly to relax bronchial smooth muscle, dilate airways, and improve airflow. This intervention directly addresses the underlying bronchospasm and helps to alleviate the acute symptoms of asthma.
B) Providing immediate rest for the client:
While rest is important in managing an acute asthma exacerbation, it is not the immediate priority. Addressing the airway obstruction with appropriate medications is crucial for stabilizing the client's condition before focusing on comfort measures such as rest.
C) Positioning the client in high-Fowler's:
Positioning the client in a high-Fowler's position can help improve lung expansion and facilitate breathing. However, this action is secondary to administering medication that can relieve the acute symptoms of bronchoconstriction. The medication should be administered first to rapidly address the exacerbation.
D) Initiating oxygen therapy:
Oxygen therapy might be necessary if the client shows signs of hypoxemia or severe respiratory distress. However, the immediate priority is to address the bronchospasm with a nebulized beta-adrenergic agonist to improve airflow. Once the acute bronchospasm is managed, oxygen therapy can be implemented if needed to support oxygen saturation.
Whether you are a student looking to ace your exams or a practicing nurse seeking to enhance your expertise , our nursing education contents will empower you with the confidence and competence to make a difference in the lives of patients and become a respected leader in the healthcare field.
Visit Naxlex, invest in your future and unlock endless possibilities with our unparalleled nursing education contents today
Report Wrong Answer on the Current Question
Do you disagree with the answer? If yes, what is your expected answer? Explain.
Kindly be descriptive with the issue you are facing.
