Related Questions
Correct Answer is D
Explanation
Choice A Reason: This choice is incorrect because administering intravenous pain medication is not the priority action for a client who has sustained partial-thickness burns. Pain medication may be indicated for pain relief and comfort, but it does not address the potential life-threatening complications of burns such as shock, infection, or respiratory distress.
Choice B Reason: This choice is incorrect because drawing blood for a CBC count is not the priority action for a client who has sustained partial-thickness burns. A CBC count may be useful to monitor the hematological status and detect any signs of infection or anemia, but it does not address the immediate needs of the client
Choice C Reason: This choice is incorrect because inserting an indwelling urinary catheter is not the priority action for a client who has sustained partial-thickness burns. A urinary catheter may be necessary to measure the urine output and assess the renal function and fluid balance, but it does not address the most urgent problem of the client.
Choice D Reason: This choice is correct because inspecting the mouth for signs of inhalation injuries is the priority action for a client who has sustained partial-thickness burns. Inhalation injuries are caused by inhaling hot air, smoke, or toxic gases that damage the airway and lungs. They can cause airway obstruction, bronchospasm, pulmonary edema, or respiratory failure. Therefore, the nurse should inspect the mouth for signs such as soot, singed nasal hairs, burns on the lips or tongue, hoarseness, stridor, or wheezes. The nurse should also monitor the oxygen saturation and arterial blood gases to assess the oxygenation and ventilation status of the client.
Correct Answer is D
Explanation
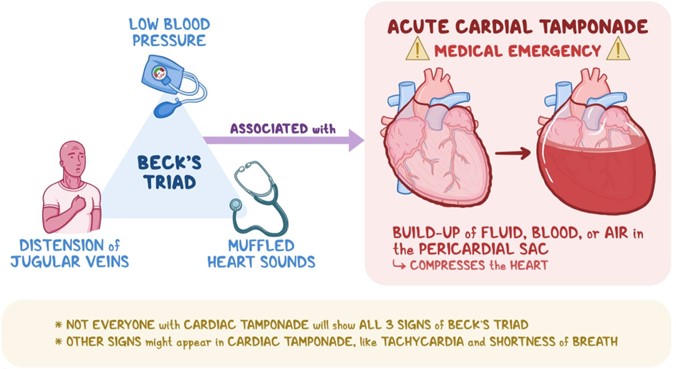
Choice A Reason: This choice is incorrect because flatened neck veins are not a sign of cardiac tamponade. Cardiac tamponade is a condition in which fluid accumulates in the pericardial sac that surrounds the heart, causing compression and impaired filling of the heart chambers. This leads to reduced cardiac output and hypotension. One of the manifestations of cardiac tamponade is distended neck veins due to increased venous pressure and impaired venous return.
Choice B Reason: This choice is incorrect because bradycardia is not a sign of cardiac tamponade. Bradycardia is a condition in which the heart rate is slower than normal (less than 60 beats per minute). It may be caused by various factors such as vagal stimulation, medication side effects, hypothyroidism, or sinus node dysfunction. It may cause symptoms such as fatigue, dizziness, or syncope, but it does not indicate cardiac tamponade.
Choice C Reason: This choice is incorrect because sudden lethargy is not a specific sign of cardiac tamponade. Lethargy is a condition in which the person feels tired, sluggish, or drowsy. It may be caused by various factors such as sleep deprivation, depression, infection, anemia, or hypoglycemia. It may affect the person's mental and physical performance, but it does not indicate cardiac tamponade.
Choice D Reason: This choice is correct because muffled heart sounds are a sign of cardiac tamponade. Muffled heart sounds are heart sounds that are fainter or softer than normal due to reduced transmission of sound waves through fluid-filled pericardial sac. They may indicate that the heart function is compromised by cardiac tamponade and require immediate intervention such as pericardiocentesis (removal of fluid from pericardial sac).