A nurse is assisting with the care of a client who is in labour and has an external electronic fetal monitor. The nurse observes that the fetal heart rate begins to decelerate after the contraction has started, with the lowest point of the deceleration occurring after the peak of the contraction. Which of the following actions should the nurse take first?
Increase the rate of the maintenance IV infusion.
Administer oxygen using a nonrebreather mask.
Elevate the client's legs.
Place the client in the lateral position.
The Correct Answer is D
Choice A rationale:
Increasing the rate of the maintenance IV infusion may be a rational action in some situations, but it is not the first priority when dealing with a fetal heart rate deceleration. The priority is to address the deceleration and potential fetal distress promptly.
Choice B rationale:
Administering oxygen using a nonrebreather mask might be beneficial for the client, but it is not the primary action to take when dealing with fetal heart rate deceleration. The priority is to address the deceleration and ensure fetal well-being.
Choice C rationale:
Elevating the client's legs is unlikely to have a significant impact on fetal heart rate deceleration. This action is more relevant in cases of maternal hypotension or when trying to improve venous return to the heart. It is not the first-line intervention for fetal heart rate decelerations.
Choice D rationale:
Placing the client in the lateral (side-lying) position is the correct action to take first. This position can help relieve pressure on the vena cava, improve blood flow, and increase oxygen supply to the fetus. By changing the client's position, the nurse can potentially resolve the fetal heart rate deceleration and improve fetal well-being.
Nursing Test Bank
Naxlex Comprehensive Predictor Exams
Related Questions
Correct Answer is A
Explanation
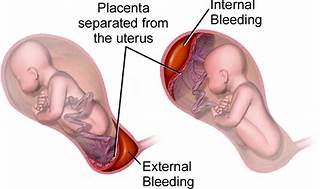
The correct answer is choice A, Maternal hypertension.
Choice A rationale:
Maternal hypertension is widely recognized as the most common risk factor for placental abruption. High blood pressure can cause the placenta to detach from the uterine wall, leading to abruption. In summary, while all the listed factors can contribute to the risk of placental abruption, maternal hypertension stands out as the most common cause, supported by multiple health sources. It’s important for nurses to recognize and manage hypertension in pregnant clients to minimize the risk of this serious complication.
Choice B rationale:
While maternal cocaine use is a significant risk factor for placental abruption due to its vasoconstrictive effects, which can compromise the placental blood flow, it is not as common as maternal hypertension.
Choice C rationale:
Maternal cigarette smoking is also a risk factor for placental abruption. Smoking can lead to a variety of complications in pregnancy, including placental problems, but again, it is less common than hypertension as a cause for abruption.
Choice D rationale:
Maternal battering can lead to trauma which may result in placental abruption. However, it is not considered the most common risk factor when compared to maternal hypertension.
Correct Answer is ["A","D","E"]
Explanation
Dysuria - Dysuria refers to painful or difficult urination. In a client with a urinary tract infection (UTI), this symptom is commonly present. The rationale behind this finding is that the infection irritates the urinary tract, causing discomfort and pain during urination. The client may experience a burning sensation or pressure while passing urine.
Choice D rationale
Hematuria - Hematuria refers to the presence of blood in the urine. In the case of a UTI, inflammation of the urinary tract can lead to tiny blood vessels rupturing, resulting in blood in the urine. This can cause the urine to appear pink, red, or brownish.
Choice E rationale:
Urinary frequency - Urinary frequency is another common symptom of a UTI. The infection can irritate the bladder lining, leading to an increased urge to urinate even when the bladder is not full. The client may feel the need to urinate frequently throughout the day and night.
Choice B rationale
Dependent edema - Dependent edema is not typically associated with a urinary tract infection. Edema is the accumulation of fluid in tissues, often causing swelling in the lower extremities due to gravity (dependent). This symptom is more commonly related to issues such as heart, kidney, or liver problems.
Choice C rationale
Polyuria - Polyuria refers to excessive urination, usually producing abnormally large volumes of urine. While frequent urination is a symptom of a UTI, polyuria, in this context, is not accurate. UTIs tend to cause frequent but smaller volumes of urine due to the irritation and inflammation of the bladder.
Whether you are a student looking to ace your exams or a practicing nurse seeking to enhance your expertise , our nursing education contents will empower you with the confidence and competence to make a difference in the lives of patients and become a respected leader in the healthcare field.
Visit Naxlex, invest in your future and unlock endless possibilities with our unparalleled nursing education contents today
Report Wrong Answer on the Current Question
Do you disagree with the answer? If yes, what is your expected answer? Explain.
Kindly be descriptive with the issue you are facing.
