A nurse is assessing a newborn following a vaginal delivery. Which of the following findings should the nurse report to the provider?
Heart rate 136/min
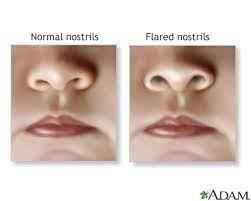
Nasal flaring
Transient strabismus
Overlapping of sutures
The Correct Answer is B
- A. Heart rate 136/min is a normal finding for a newborn. The normal range of heart rate for a newborn is 100 to 160/min.
- B. Nasal flaring is an abnormal finding for a newborn. Nasal flaring indicates respiratory distress and may be caused by conditions such as pneumonia, meconium aspiration, or congenital heart defects.
- C. Transient strabismus is a normal finding for a newborn. Transient strabismus is a temporary misalignment of the eyes that occurs due to weak eye muscles and poor coordination. It usually resolves by 3 to 6 months of age.
- D. Overlapping of sutures is a normal finding for a newborn. Overlapping of sutures is caused by molding of the skull during delivery and allows the head to fit through the birth canal. It usually resolves within a few days after birth.
Nursing Test Bank
Naxlex Comprehensive Predictor Exams
Related Questions
Correct Answer is D
Explanation
Choice A rationale:
Taking corrective measures to enforce hand hygiene should not be the first step. It is important to establish a baseline and understand the current situation through data collection and analysis before implementing corrective measures.
Choice B rationale:
Establishing methods for collecting data within the facility is a crucial first step. Gathering information about the current hand hygiene practices, compliance rates, and areas of improvement is essential for the audit process. Data collection provides a factual basis for identifying problems and implementing targeted interventions.
Choice C rationale:
Comparing the facility's data with the established criteria for hand hygiene is a subsequent step after data collection. This step helps in evaluating the current practices against the accepted standards and guidelines. However, it is not the first step in the audit process.
Choice D rationale:
Determining the accepted standards for hand hygiene is an essential first step. It involves researching and understanding the national and international guidelines, protocols, and recommendations related to hand hygiene. Knowing the standards helps the task force establish a benchmark against which the facility's practices can be evaluated. It provides a foundation for data collection and subsequent analysis.
Correct Answer is C
Explanation
Choice A rationale:
This statement implies that the nurse attempted the dressing change but was unsuccessful. However, the information about the dressing not being soiled is irrelevant to the incident report. The key issue is the omission of the prescribed procedure.
Choice B rationale:
This statement acknowledges the omission but lacks specificity. It does not state the nature of the omission or the potential consequences, making it less informative for future prevention strategies.
Choice C rationale:
This statement clearly and concisely states the situation, indicating that the prescribed dressing change was omitted. It provides essential information for understanding what happened, allowing for appropriate investigation and preventive measures.
Choice D rationale:
This statement confirms the completion of the incident report but does not provide details about the incident itself. Without specific information about the omission, this statement is insufficient for understanding the nature of the error and implementing preventive actions.
Whether you are a student looking to ace your exams or a practicing nurse seeking to enhance your expertise , our nursing education contents will empower you with the confidence and competence to make a difference in the lives of patients and become a respected leader in the healthcare field.
Visit Naxlex, invest in your future and unlock endless possibilities with our unparalleled nursing education contents today
Report Wrong Answer on the Current Question
Do you disagree with the answer? If yes, what is your expected answer? Explain.
Kindly be descriptive with the issue you are facing.
