A nurse is assessing a client who is experiencing an anaphylactic reaction to an antibiotic. Which of the following manifestations of anaphylaxis should the nurse expect?
Hypertonic reflexes
increase in systolic blood pressure
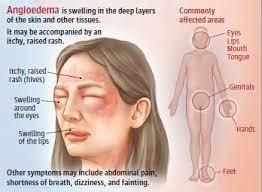
Angioedema
Urinary retention
The Correct Answer is C
The nurse should expect angioedema as one of the manifestations of anaphylaxis in a client experiencing an allergic reaction to an antibiotic. Angioedema is a severe swelling that occurs beneath the skin, typically affecting the face, lips, tongue, throat, or other body parts. It is a result of the release of histamine and other inflammatory mediators in response to the allergen.
Anaphylaxis is a life-threatening allergic reaction that can occur rapidly and affect multiple body systems. In addition to angioedema, other common manifestations of anaphylaxis include:
-
Difficulty breathing or wheezing due to bronchospasm
-
Hives or urticaria, which are itchy raised skin rashes
-
Severe itching or tingling sensation
-
Rapid and weak pulse
-
Low blood pressure leading to hypotension
-
Nausea, vomiting, or diarrhea
-
Feeling of impending doom or anxiety
Let's go through the other options:
A. Hypertonic reflexes: This is not a manifestation of anaphylaxis. "Hypertonic reflexes" are not typically associated with allergic reactions or anaphylaxis. Hypertonic reflexes refer to increased muscle tone, but they are not part of the usual presentation of anaphylaxis.
B. Increase in systolic blood pressure: Anaphylaxis usually leads to a decrease in blood pressure rather than an increase. The decrease in blood pressure can be severe and result in shock, which is a life-threatening condition.
D. Urinary retention: Urinary retention is not a common manifestation of anaphylaxis. Anaphylaxis primarily affects the respiratory and circulatory systems, leading to airway constriction, difficulty breathing, and cardiovascular collapse. Urinary retention is not directly related to the pathophysiology of anaphylaxis.
Nursing Test Bank
Naxlex Comprehensive Predictor Exams
Related Questions
Correct Answer is C
Explanation
Smoking is a known risk factor for the development of aspirin-induced ulcers. It can increase the risk of gastrointestinal bleeding and compromise the integrity of the gastric mucosa. Smoking can also impair the healing process and increase the risk of complications associated with ulcers.
While the other factors mentioned in the options may have their own health implications, smoking is specifically associated with an increased risk of aspirin-induced ulcers. Therefore, the nurse should identify the client's smoking habit as a risk factor for the development of an aspirin-induced ulcer.
Correct Answer is D
Explanation
When planning care for a client who had a myocardial infarction and is receiving thrombolytic therapy with an IV infusion of alteplase, the nurse should include the intervention of monitoring for changes in the client's level of consciousness.
Alteplase is a thrombolytic medication used to break down blood clots in certain medical emergencies, such as acute myocardial infarction (heart attack) or ischemic stroke. One of the potential complications of thrombolytic therapy, including alteplase, is bleeding. The medication's action of breaking down blood clots can also affect the body's natural clotting mechanisms, increasing the risk of bleeding.
Bleeding in the brain is a severe and potentially life-threatening complication associated with thrombolytic therapy. Therefore, it is essential for the nurse to closely monitor the client for any signs of intracranial bleeding, such as changes in the level of consciousness, confusion, severe headache, slurred speech, or weakness on one side of the body.
Let's go through the other options:
A. Administer aspirin instead of acetaminophen for fever: While aspirin is commonly used in the management of myocardial infarction, it is not specifically indicated for fever. Acetaminophen is the preferred antipyretic medication for fever management in most cases, and it does not interfere with the action of thrombolytic therapy.
B. Ambulate the client as often as tolerated: While early ambulation is beneficial for clients with myocardial infarction, it may not be appropriate during thrombolytic therapy. Thrombolytic therapy carries an increased risk of bleeding, and ambulation may be limited or contraindicated during the treatment period, depending on the client's overall condition and bleeding risk.
C. Administer a sodium phosphate enema for constipation: The administration of a sodium phosphate enema is not a specific intervention related to thrombolytic therapy or myocardial infarction. Bowel management is important for client comfort and overall well-being, but it is not a priority intervention in the immediate care of a client undergoing thrombolytic therapy.
Whether you are a student looking to ace your exams or a practicing nurse seeking to enhance your expertise , our nursing education contents will empower you with the confidence and competence to make a difference in the lives of patients and become a respected leader in the healthcare field.
Visit Naxlex, invest in your future and unlock endless possibilities with our unparalleled nursing education contents today
Report Wrong Answer on the Current Question
Do you disagree with the answer? If yes, what is your expected answer? Explain.
Kindly be descriptive with the issue you are facing.
