A patient has been diagnosed with septic shock.
What collaborative interventions would be expected? (Select all that apply)
Temperature control for either hypothermia or hyperthermia.
Administration of cardiotonic agents such as dopamine, dobutamine, or norepinephrine.
Administration of a thrombolytic (streptokinase).
Subcutaneous administration of epinephrine (1:1000) 0.5 to 1 ml every 5 to 15 minutes.
Blood cultures from all suspected sources before administration of antibiotics.
Vigorous intravenous fluid resuscitation with 0.9% sodium chloride.
Correct Answer : A,B,E,F
Choice A rationale:
Temperature control for either hypothermia or hyperthermia is crucial in septic shock management. Here's a detailed explanation:
Hypothermia:
Mechanism: Septic shock often causes impaired thermoregulation, leading to hypothermia. It can worsen shock by decreasing cardiac output, impairing coagulation, and promoting vasoconstriction.
Intervention: Active warming measures are essential, including: External warming devices (e.g., blankets, forced air warmers) Intravenous fluids warmed to 39-42°C
Warmed humidified oxygen
Minimizing exposure and covering the patient Hyperthermia:
Mechanism: Sepsis can trigger an excessive inflammatory response, leading to hyperthermia. It can exacerbate tissue injury, increase metabolic demands, and worsen organ dysfunction.
Intervention: Aggressive measures to lower temperature are necessary, including:
Antipyretic medications (e.g., acetaminophen, ibuprofen) External cooling methods (e.g., cooling blankets, ice packs) Sedation if shivering occurs
Choice B rationale:
Administration of cardiotonic agents such as dopamine, dobutamine, or norepinephrine is often required in septic shock to: Improve cardiac output: These agents increase myocardial contractility and heart rate, enhancing blood flow to vital organs.
Maintain blood pressure: They support vasoconstriction, counteracting the widespread vasodilation characteristic of septic shock.
Improve tissue perfusion: By optimizing cardiac output and blood pressure, they help ensure adequate oxygen and nutrient delivery to tissues.
Choice E rationale:
Blood cultures from all suspected sources before administration of antibiotics are essential for guiding appropriate antibiotic therapy.
Early identification of the causative organism: This information is crucial for selecting the most effective antibiotic regimen.
Prevention of antibiotic resistance: Judicious use of antibiotics based on culture results helps prevent the development of antibiotic-resistant bacteria.
Choice F rationale:
Vigorous intravenous fluid resuscitation with 0.9% sodium chloride is a cornerstone of septic shock management.
Replenishing intravascular volume: Septic shock often causes profound intravascular volume depletion due to capillary leak and vasodilation. Fluid resuscitation aims to restore circulating volume and maintain organ perfusion.
Improving hemodynamic stability: By increasing preload and cardiac output, fluids help stabilize blood pressure and support vital organ function.
Nursing Test Bank
Naxlex Comprehensive Predictor Exams
Related Questions
Correct Answer is C
Explanation
Choice A rationale:
Bilateral flank pain is not a typical sign of an allergic blood transfusion reaction. It can be associated with other conditions, such as kidney problems, musculoskeletal issues, or abdominal aortic aneurysm. While it's important to assess flank pain, it doesn't directly suggest an allergic reaction to the transfusion.
Choice B Rationale:
Distended jugular veins can indicate fluid overload, which could potentially occur during a transfusion. However, it's not a specific sign of an allergic reaction. Fluid overload can result from various causes, including heart failure, kidney problems, or excessive fluid intake. It's crucial to monitor for fluid overload during transfusions, but it doesn't definitively point to an allergic reaction.
Choice C Rationale:
Generalized urticaria, or hives, is a hallmark sign of an allergic reaction. It's characterized by raised, red, itchy welts that can appear on various parts of the body. Hives can develop rapidly and spread extensively. During a blood transfusion, generalized urticaria strongly suggests that the patient's immune system is reacting to a component of the transfused blood, such as proteins or antibodies.
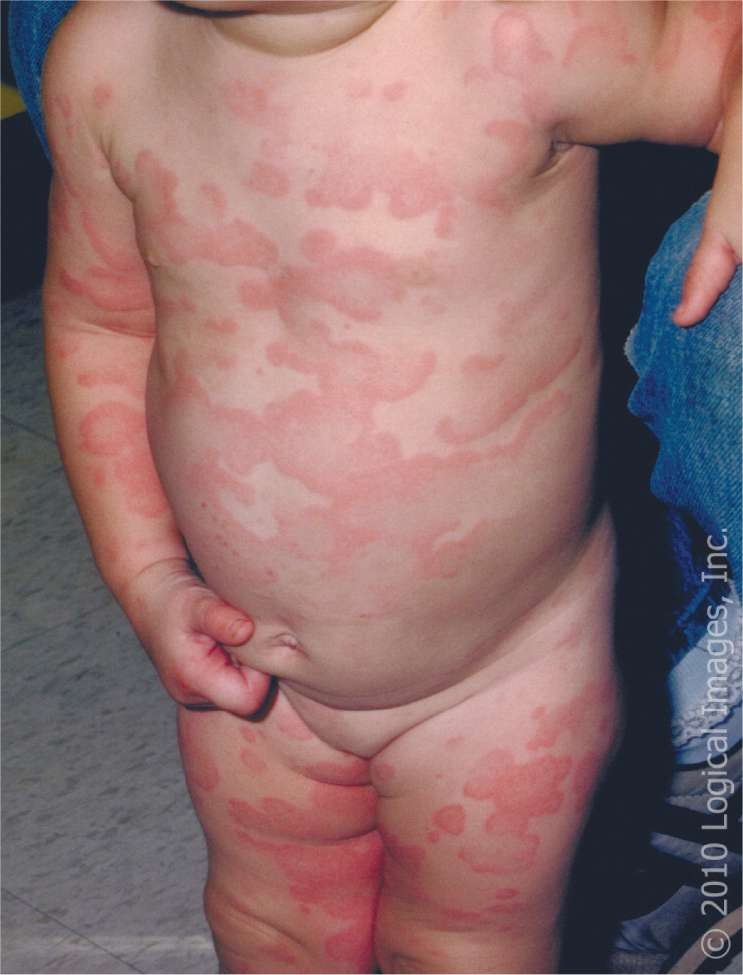
Choice D Rationale:
Blood pressure 184/92 mm Hg is elevated and could be concerning, but it's not specific to allergic reactions. High blood pressure can have various causes, including stress, pain, anxiety, or underlying hypertension. While monitoring blood pressure during transfusions is essential, it doesn't directly indicate an allergic reaction.
Correct Answer is B
Explanation
Choice A rationale:
While explaining the importance and rationale of the new policy may be helpful in some cases, it may not be sufficient for nurses who are resistant to change. This approach assumes that the nurse's resistance is due to a lack of understanding, which may not be the case. It's possible that the nurse understands the rationale but has other concerns or objections.
Focusing solely on explaining the rationale can make the nurse feel they are not being listened to or that their concerns are not being valued. This can further contribute to resistance.
Choice B rationale:
Encouraging the nurse to verbalize their reasons for resistance allows the nurse manager to understand the root cause of the resistance. This could include:
Concerns about the effectiveness of the new policy
Belief that the new policy will create more work or make their job more difficult
Feeling that they were not adequately consulted or involved in the decision-making process Personal factors such as fear of change or a preference for established routines
Once the nurse manager understands the nurse's concerns, they can work together to address them and find ways to facilitate acceptance of the new policy. This approach fosters open communication, collaboration, and shared decision-making, which are essential for successful change management.
Choice C rationale:
Indicating disciplinary consequences may be necessary in some cases, but it should be a last resort. It can create a negative and hostile work environment, further alienate the nurse, and potentially lead to resentment and decreased morale among other staff members.
It's important to prioritize understanding and addressing the underlying reasons for resistance before resorting to disciplinary measures.
Choice D rationale:
Ignoring the resistance and relying on peer pressure is a passive and ineffective approach. It does not address the nurse's concerns and may even exacerbate the situation. This can lead to conflict among staff members, create a divide between those who support the change and those who resist it, and potentially compromise patient care.
Whether you are a student looking to ace your exams or a practicing nurse seeking to enhance your expertise , our nursing education contents will empower you with the confidence and competence to make a difference in the lives of patients and become a respected leader in the healthcare field.
Visit Naxlex, invest in your future and unlock endless possibilities with our unparalleled nursing education contents today
Report Wrong Answer on the Current Question
Do you disagree with the answer? If yes, what is your expected answer? Explain.
Kindly be descriptive with the issue you are facing.
