A patient complains of worsening nasal congestion despite the use of oxymetazoline (Afrin) nasal spray every 2 to 4 hours for the past 5 days. The nurse's response is based on the knowledge that
Oxymetazoline should be administered in an hourly regimen for severe congestion.
Oxymetazoline is not an effective nasal decongestant
Sustained use of nasal decongestants over several days may result in rebound congestion
The patient is probably displaying an idiosyncratic reaction to oxymetazoline
The Correct Answer is C
Rebound congestion, also known as rhinitis medicamentosa, is a common adverse effect associated with the prolonged use of nasal decongestants. It occurs when the blood vessels in the nasal passages become dependent on the medication for constriction and lose their ability to regulate naturally. As a result, when the medication wears off, the nasal congestion worsens, leading to a cycle of continued use and worsening symptoms.
In this scenario, the patient's complaint of worsening nasal congestion despite using oxymetazoline every 2 to 4 hours for the past 5 days suggests the possibility of rebound congestion. The nurse should explain to the patient that prolonged or frequent use of nasal decongestants can lead to this effect and recommend gradually tapering off the medication use or discontinuing it altogether. The nurse may also suggest alternative non-medication strategies for managing nasal congestion, such as saline nasal sprays or steam inhalation.
Nursing Test Bank
Naxlex Comprehensive Predictor Exams
Related Questions
Correct Answer is D
Explanation
Montelukast is typically prescribed as a once-daily medication for the treatment of asthma. Taking it in the evening can be beneficial as it helps to control asthma symptoms throughout the day and night. It is important to follow the prescribed dosing schedule provided by the healthcare provider.
The other statements mentioned are incorrect:
A. "I'll rinse my mouth after taking this medication": Rinsing the mouth after taking montelukast is not necessary as it is not an inhaled medication. Rinsing the mouth is typically recommended after using inhaled corticosteroids to reduce the risk of oral thrush.
B. "I'll take this medication when I get an asthma attack": Montelukast is a long-term control medication used to prevent asthma attacks and manage chronic asthma symptoms. It is not intended for immediate relief during an asthma attack.
C. "I use a spacer device when I inhale this medication": Montelukast is not an inhaled medication, so the use of a spacer device is not applicable. Spacer devices are commonly used with inhaled medications to improve the delivery of the medication to the lungs.
Correct Answer is A
Explanation
Traditional antihistamines like diphenhydramine are known to have sedating properties, which can cause drowsiness and impair cognitive function. On the other hand, loratadine is classified as a non-sedating or second-generation antihistamine. It is designed to have less of a sedative effect, allowing individuals to take it during the day without experiencing significant drowsiness or impairment.
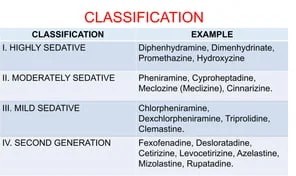
It is important to note that individual responses to medications can vary, and some individuals may still experience mild drowsiness with loratadine. However, compared to diphenhydramine, loratadine is generally associated with a lower risk of sedation.
Whether you are a student looking to ace your exams or a practicing nurse seeking to enhance your expertise , our nursing education contents will empower you with the confidence and competence to make a difference in the lives of patients and become a respected leader in the healthcare field.
Visit Naxlex, invest in your future and unlock endless possibilities with our unparalleled nursing education contents today
Report Wrong Answer on the Current Question
Do you disagree with the answer? If yes, what is your expected answer? Explain.
Kindly be descriptive with the issue you are facing.
