A nurse is reinforcing teaching with a client about advance directives and a health care proxy.
Which of the following client statements indicates an understanding of the teaching?
Once my health care proxy is in place, I relinquish my right to make my own decisions.
If I have a health care proxy, then I do not need to have a living will.
My health care proxy designee is not able to sign a consent form on my behalf.
I do not need to name a relative as my designee in my health care proxy.
None
None
The Correct Answer is D
A. Having a health care proxy does not mean that the individual relinquishes their right to make their own decisions. A health care proxy is designated to make decisions on behalf of the individual when they are unable to do so, but the individual retains the right to make decisions if they are capable.
B. Having a health care proxy does not eliminate the need for a living will. A living will outline the individual's specific wishes regarding medical treatments and end-of-life care, while a health care proxy designates a person to make decisions on their behalf. Both documents serve different purposes and can work together to ensure the individual's wishes are respected.
C. A health care proxy designee is typically empowered to make medical decisions on your behalf, including signing consent forms if necessary. This is one of the primary roles of a health care proxy – to act in your best interests when you are unable to make decisions yourself, including signing forms for procedures or treatments.
D. The individual has the choice to name any person as their health care proxy designee, regardless of their relationship. It is important to choose someone who understands the individual's wishes and can make decisions in their best interest. The decision of whom to name as the health care proxy designee is personal and should be based on trust and understanding.
Nursing Test Bank
Naxlex Comprehensive Predictor Exams
Related Questions
Correct Answer is D
Explanation
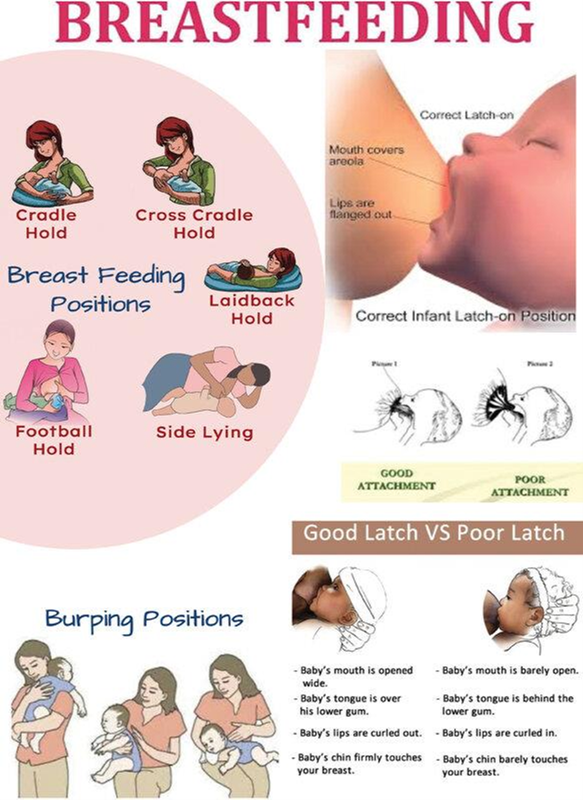
Having the baby latch on to both the nipple and areola during breastfeeding is essential for effective milk transfer and optimal breastfeeding. The baby should take in a good portion of the areola along with the nipple to ensure a proper latch and a comfortable feeding experience for both the mother and the baby. This allows the baby to obtain enough milk and stimulates milk production in the mother.
Let's briefly discuss the other statements:
A- "My baby should breastfeed 5 to 10 minutes on each breast": The duration of breastfeeding can vary from baby to baby, but it is generally recommended to allow the baby to breastfeed until they are satisfied and have emptied one breast before switching to the other breast. This ensures that the baby receives both the foremilk and the hindmilk, which are important for adequate nutrition.
B- "I should not wake my baby during the night to breastfeed": In the early days after birth, it is important to establish frequent and regular breastfeeding to support milk production and ensure the baby receives enough nourishment. Newborns typically need to breastfeed at least 8 to 12 times in 24 hours, including during the night. If the baby is sleeping for a long period, it may be necessary to wake them for feeding to ensure proper nutrition and hydration.
C- "I should keep my baby on a strict feeding schedule": Breastfeeding should be based on the baby's cues and demand rather than a strict schedule. Newborns should be breastfed whenever they show hunger signs, such as rooting, sucking motions, or increased alertness. This helps establish a good milk supply and allows the baby to feed according to their individual needs.
Correct Answer is B
Explanation
Correct answer: B
A. Place no more than one small pillow in the crib
The American Academy of Pediatrics (AAP) recommends that infants should sleep on a firm and flat surface without any pillows, blankets, or soft bedding. These items can pose a suffocation risk.So, the nurse should advise against using any pillows in the crib.
B. This is agood recommendation. Bibs can be a choking hazard during sleep.Removing them ensures the baby’s safety and reduces the risk of accidental suffocation
C. Making sure the crib mattress is soft in (option C) is not recommended. The crib mattress should be firm to provide a safe sleeping surface for the infant. Soft mattresses can increase the risk of suffocation.
D. Starting to use a highchair for feedings at 3 months old in (option D) is not typically necessary or developmentally appropriate. At this age, infants are typically fed while being held in a caregiver's arms or in a reclined position, such as in a baby bouncer or supported seat.
Whether you are a student looking to ace your exams or a practicing nurse seeking to enhance your expertise , our nursing education contents will empower you with the confidence and competence to make a difference in the lives of patients and become a respected leader in the healthcare field.
Visit Naxlex, invest in your future and unlock endless possibilities with our unparalleled nursing education contents today
Report Wrong Answer on the Current Question
Do you disagree with the answer? If yes, what is your expected answer? Explain.
Kindly be descriptive with the issue you are facing.
