A nurse is performing a Weber test on a client who reports difficulty hearing in his left ear. The client informs the nurse that he can hear the tone louder in his left ear. Which of the following does this result indicate?
The test is inconclusive
The client has conductive hearing loss
The client has normal hearing
The client has sensorineural hearing loss
The Correct Answer is B
Choice A Reason: The test is not inconclusive, but rather positive for conductive hearing loss. The Weber test involves placing a vibrating tuning fork on the center of the forehead and asking the client which ear hears the sound louder. It can help differentiate between conductive and sensorineural hearing loss.
Choice B Reason: This is the correct choice. The client has conductive hearing loss, which is a type of hearing loss that occurs when sound waves are blocked or reduced in the outer or middle ear. It can be caused by earwax, infection, fluid, perforation, or trauma. In conductive hearing loss, the Weber test shows lateralization to the affected ear, meaning the sound is heard louder in that ear.
Choice C Reason: The client does not have normal hearing, but rather conductive hearing loss. In normal hearing, the Weber test shows no lateralization, meaning the sound is heard equally in both ears.
Choice D Reason: The client does not have sensorineural hearing loss, but rather conductive hearing loss. Sensorineural hearing loss is a type of hearing loss that occurs when there is damage to the inner ear or auditory nerve. It can be caused by aging, noise exposure, disease, or drugs. In sensorineural hearing loss, the Weber test shows lateralization to the unaffected ear, meaning the sound is heard louder in that ear.
Nursing Test Bank
Naxlex Comprehensive Predictor Exams
Related Questions
Correct Answer is B
Explanation
Choice A reason: This is incorrect because allergies are not a risk factor for developing Barrett's esophagus. Allergies are hypersensitive reactions of the immune system to certain substances, such as pollen, dust, or food. They can cause symptoms such as sneezing, itching, or hives, but they do not affect the esophagus or stomach acid.
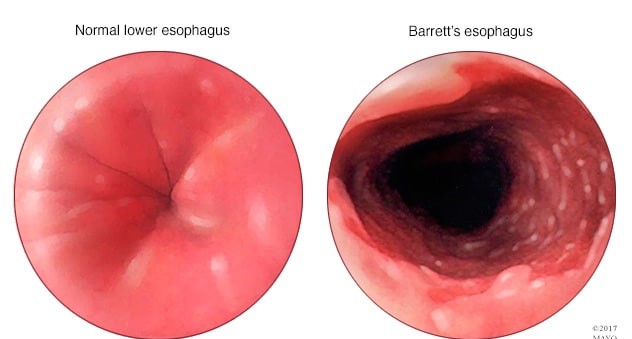
Choice B reason: This is the correct answer because gastroesophageal reflux disorder (GERD) is the most common risk factor for developing Barrett's esophagus. GERD is a condition where the lower esophageal sphincter (LES) does not close properly and allows stomach acid to flow back into the esophagus. This can cause inflammation, irritation, and damage to the esophageal lining. Over time, this can lead to changes in the cells of the esophagus, which is called Barrett's esophagus.
Choice C reason: This is incorrect because being a vegetarian is not a risk factor for developing Barrett's esophagus. Being a vegetarian means avoiding meat and animal products in the diet. This can have health benefits such as lower cholesterol and blood pressure levels, but it does not affect the esophagus or stomach acid.
Choice D reason: This is incorrect because Barrett's esophagus is not a genetic condition that one is born with. Barrett's esophagus is an acquired condition that results from chronic exposure to stomach acid in the esophagus. It is not inherited from one's parents or passed on to one's children.
Correct Answer is ["D","E"]
Explanation
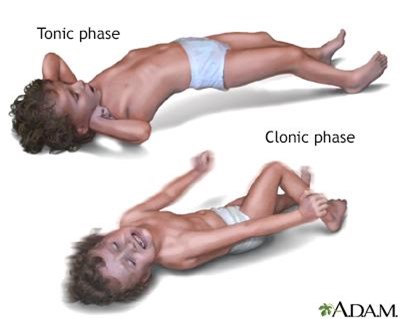
Choice A Reason: This choice is incorrect. Placing the client into a supine position is not an action that the nurse should take, as it can compromise the airway and increase the risk of aspiration. The nurse should position the client on their side with their head tilted slightly forward to allow saliva and secretions to drain out of their mouth.
Choice B Reason: This choice is incorrect. Applying restraints is not an action that the nurse should take, as it can cause injury and increase agitation. The nurse should protect the client from harm by removing any objects or furniture that may cause harm and padding any hard surfaces with blankets or pillows.
Choice C Reason: This choice is incorrect. Inserting a bite stick into the client's mouth is not an action that the nurse should take, as it can cause injury and obstruction. The nurse should never force anything into the client's mouth during a seizure, as it can damage their teeth, gums, tongue, or jaw.
Choice D Reason: This is a correct choice. Loosening restrictive clothing is an action that the nurse should take, as it can improve breathing and circulation. The nurse should unbutton any tight collars, belts, or ties that may constrict the chest or neck.
Choice E Reason: This is a correct choice. Placing a pillow under the client's head is an action that the nurse should take, as it can prevent injury and provide comfort. The nurse should support the client's head with a soft pillow or cushion to prevent hitting it against any hard surfaces.
Whether you are a student looking to ace your exams or a practicing nurse seeking to enhance your expertise , our nursing education contents will empower you with the confidence and competence to make a difference in the lives of patients and become a respected leader in the healthcare field.
Visit Naxlex, invest in your future and unlock endless possibilities with our unparalleled nursing education contents today
Report Wrong Answer on the Current Question
Do you disagree with the answer? If yes, what is your expected answer? Explain.
Kindly be descriptive with the issue you are facing.
