A nurse is observing an assistive personnel (AP). For which of the following actions by the AP should the nurse intervene?
Logs off the computer after entering a client's intake and output totals.
Tears a document with client information in half before disposing of it in a waste basket.
Denies a request by another AP to use her password to enter client's vital signs.
Removes a clipboard with client information from the room during visiting hours.
The Correct Answer is B
The nurse should intervene when the AP tears a document with client information in half before disposing of it in a waste basket. This is because client information is confidential and should be disposed of properly to protect the client's privacy. Tearing a document in half is not sufficient to ensure that the information is protected.
Option A is incorrect because logging off the computer after entering a client's intake and output totals is an appropriate action.
Option C is incorrect because denying a request by another AP to use her password to enter the client's vital signs is an appropriate action to protect the client's information.
Option D is incorrect because removing a clipboard with client information from the room during visiting hours may be necessary to protect the client's privacy.
Nursing Test Bank
Naxlex Comprehensive Predictor Exams
Related Questions
Correct Answer is C
Explanation
An incident report should be filed whenever an unexpected event occurs. The rule of thumb is that any time a patient makes a complaint, a medication error occurs, a medical device malfunctions, or anyone— patient, staff member, or visitor—is injured or involved in a situation with the potential for injury, an incident report is required ⁴. In this case, the client's missing dentures would be considered a complaint and would require the nurse to complete an incident report.
The other options do not require an incident report. Disagreeing with the nurse manager about inadequate staffing [a], a staff member not arriving at the facility to work an assigned shift [b], and discovering that the client does not have advanced directives [d] are not situations that would require an incident report according to the information provided in my sources.
Correct Answer is D
Explanation
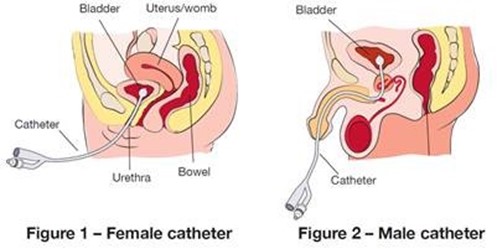
If a client is concerned about her privacy during a urinary catheterization procedure, the nurse should close the door and cover the client during the procedure. This action helps to maintain the client's privacy and dignity.
Option A may also be helpful in alleviating the client's concern by providing information about the procedure.
Option B may also be helpful in ensuring that the procedure is performed efficiently.
Option C may not be necessary if the client is not resistant to the procedure.
Whether you are a student looking to ace your exams or a practicing nurse seeking to enhance your expertise , our nursing education contents will empower you with the confidence and competence to make a difference in the lives of patients and become a respected leader in the healthcare field.
Visit Naxlex, invest in your future and unlock endless possibilities with our unparalleled nursing education contents today
Report Wrong Answer on the Current Question
Do you disagree with the answer? If yes, what is your expected answer? Explain.
Kindly be descriptive with the issue you are facing.
