A nurse is evaluating the laboratory findings of a client who has wound dehiscence following abdominal surgery. Which of the following findings should indicate to the nurse that the client is experiencing fluid volume deficit?
Potassium 3.5 mEq/L
Sodium 145 mEq/L
Hematocrit 53%
HbA1c 5%
The Correct Answer is C
Choice A reason: Potassium 3.5 mEq/L is not a finding that indicates fluid volume deficit because it is within the normal range, which is 3.5 to 5.0 mEq/L. Potassium is an electrolyte that regulates nerve and muscle function, acid-base balance, and fluid balance. Potassium level can be affected by various factors, such as diet, medication, kidney function, and dehydration.
Choice B reason: Sodium 145 mEq/L is not a finding that indicates fluid volume deficit because it is within the normal range, which is 136 to 145 mEq/L. Sodium is an electrolyte that regulates blood pressure, blood volume, and fluid balance. Sodium level can be affected by various factors, such as diet, medication, kidney function, and fluid loss.
Choice C reason: Hematocrit 53% is a finding that indicates fluid volume deficit because it is above the normal range, which is 38 to 50% for men and 34 to 46% for women. Hematocrit is the percentage of red blood cells in the total blood volume. Hematocrit level can increase due to dehydration, which causes hemoconcentration or increased blood viscosity.
Choice D reason: HbA1c 5% is not a finding that indicates fluid volume deficit because it is within the normal range, which is less than 5.7%. HbA1c is the percentage of hemoglobin that is attached to glucose. HbA1c level reflects the average blood glucose level over the past two to three months. HbA1c level can be affected by various factors, such as diabetes, anemia, and medication.
Nursing Test Bank
Naxlex Comprehensive Predictor Exams
Related Questions
Correct Answer is B
Explanation
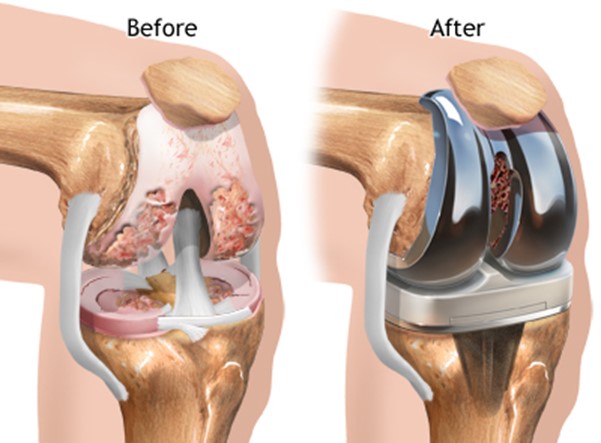
Choice A reason: Applying ice packs for 15 minutes every hour is not an effective intervention for managing edema following knee replacement surgery because it can impair blood circulation and delay healing. Ice packs can also cause frostbite or nerve damage if applied for too long or too frequently. Ice packs should be used only for the first 24 to 48 hours after surgery and with a cloth barrier between the skin and the ice.
Choice B reason: Elevating the affected leg above the heart level is an effective intervention for managing edema following knee replacement surgery because it can reduce swelling and pain by facilitating venous return and lymphatic drainage. Elevation can also prevent blood clots and infection by improving blood flow and oxygen delivery to the wound site.
Choice C reason: Consuming nutrition-dense foods first is not a relevant intervention for managing edema following knee replacement surgery because it does not directly affect fluid balance or wound healing. Nutrition-dense foods are those that provide high amounts of nutrients per serving, such as eggs, cheese, nuts, beans, and meat. Nutrition-dense foods are important for overall health, but not specifically for edema management.
Choice D reason: Wearing compression stockings during the day is not a recommended intervention for managing edema following knee replacement surgery because it can interfere with wound healing and increase the risk of infection. Compression stockings can also cause skin irritation, blisters, or ulcers if worn incorrectly or too tightly. Compression stockings should be avoided until the wound is fully healed and only used under medical supervision.
Correct Answer is D
Explanation
Choice A reason: Hemoglobin 16 g/dL is within the normal range for adults and does not indicate an adverse effect of TPN.
Choice B reason: Temperature 36.1°C (97°F) is normal and does not indicate an infection or inflammation, which are possible complications of TPN.
Choice C reason: Blood glucose 98 mg/dL is normal and does not indicate hyperglycemia or hypoglycemia, which are common problems associated with TPN.
Choice D reason: Weight gain of 1.5 kg (3 lB. per day is excessive and indicates fluid overload, which can result from too rapid or too high infusion of TPN. Fluid overload can cause edema, hypertension, heart failure, and pulmonary congestion.
Whether you are a student looking to ace your exams or a practicing nurse seeking to enhance your expertise , our nursing education contents will empower you with the confidence and competence to make a difference in the lives of patients and become a respected leader in the healthcare field.
Visit Naxlex, invest in your future and unlock endless possibilities with our unparalleled nursing education contents today
Report Wrong Answer on the Current Question
Do you disagree with the answer? If yes, what is your expected answer? Explain.
Kindly be descriptive with the issue you are facing.
