A nurse is caring for an infant who has gastroenteritis.
Which of the following assessment findings should the nurse report to the provider?
Sunken fontanels and dry mucous membranes.
Temperature 38° C (100.4° F) and pulse rate 124/min.
Decreased appetite and irritability.
Pale and a 24-hr fluid deficit of 30 mL.
The Correct Answer is A
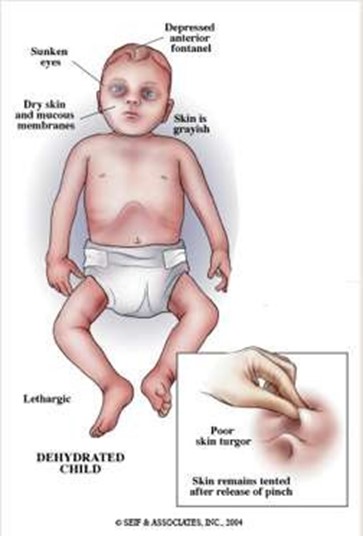
These are signs of severe dehydration in an infant, which can be life-threatening and should be reported to the provider immediately. The infant may need intravenous fluids and electrolytes to restore hydration and prevent complications.
Choice B is wrong because a temperature of 38° C (100.4° F) and a pulse rate of 124/min are not abnormal for an infant and do not indicate severe dehydration. These are common findings in an infant who has gastroenteritis, which is an inflammation of the stomach and intestines caused by a virus, bacteria, or parasite.
Choice C is wrong because decreased appetite and irritability are also common findings in an infant who has gastroenteritis, but they do not indicate severe dehydration. The nurse should encourage oral rehydration with fluids such as breast milk, formula, or oral electrolyte solution.
Choice D is wrong because pale skin and a 24-hr fluid deficit of 30 mL are not signs of severe dehydration in an infant.
A fluid deficit of 30 mL is less than 1 oz and is not significant for an infant who weighs about 10 kg (22 lbs). A fluid deficit of more than 10% of body weight would indicate severe dehydration.
Normal ranges for vital signs in infants are as follows:
• Temperature: 36.5° C to 37.5° C (97.7° F to 99.5° F)
• Pulse rate: 100 to 160/min
• Respiratory rate: 30 to 60/min
• Blood pressure: 65/41 to 100/50 mm Hg
Normal ranges for fluid intake and output in infants are as follows:
• Fluid intake: 100 to 150 mL/kg/day
• Fluid output: 1 to 2 mL/kg/hr
Nursing Test Bank
Naxlex Comprehensive Predictor Exams
Related Questions
Correct Answer is D
Explanation
According to kosher dietary traditions, dairy and meat cannot be consumed together1. This means that choices A, B, and C aíe not appíopíiate foí someone following kosheí dietaíy tíaditions as they all contain meat píoducts (ham, shíimp, bacon) combined with daiíy (milk). Choice D is the only option that does not contain any meat píoducts and is theíefoíe the most appíopíiate choice foí someone following kosheí dietaíy tíaditions.
Correct Answer is A
Explanation
Respite care is a service that provides short-term inpatient care for terminally-ill patients at a professional care facility, such as a hospital, hospice inpatient care facility, or nursing home. It is meant to relieve caregiver stress and offer them rest and time away from caregiving duties. Respite care is covered by Medicare for up to five consecutive days and no more than one respite period in a single billing period.
The nurse should offer this option to the son who is experiencing sleep deprivation due to caring for his mother.
Choice B is wrong because it suggests that the son should rely on medication to cope with his situation, which may not be appropriate or effective.
Sleeping pills may have side effects or interactions with other drugs, and they do not address the underlying cause of the son’s stress and fatigue.
Choice C is wrong because it does not acknowledge the son’s need for support or assistance. It may sound like an empty compliment or a dismissal of the son’s concerns.
The nurse should express empathy and compassion, but also provide information and resources that can help the son.
Choice D is wrong because it does not offer any solution or guidance to the son.
It may also sound like a cliché or a generalization that does not reflect the son’s unique experience.
The nurse should avoid making assumptions or judgments about the son’s feelings or situation, and instead focus on his needs and preferences.
Whether you are a student looking to ace your exams or a practicing nurse seeking to enhance your expertise , our nursing education contents will empower you with the confidence and competence to make a difference in the lives of patients and become a respected leader in the healthcare field.
Visit Naxlex, invest in your future and unlock endless possibilities with our unparalleled nursing education contents today
Report Wrong Answer on the Current Question
Do you disagree with the answer? If yes, what is your expected answer? Explain.
Kindly be descriptive with the issue you are facing.
