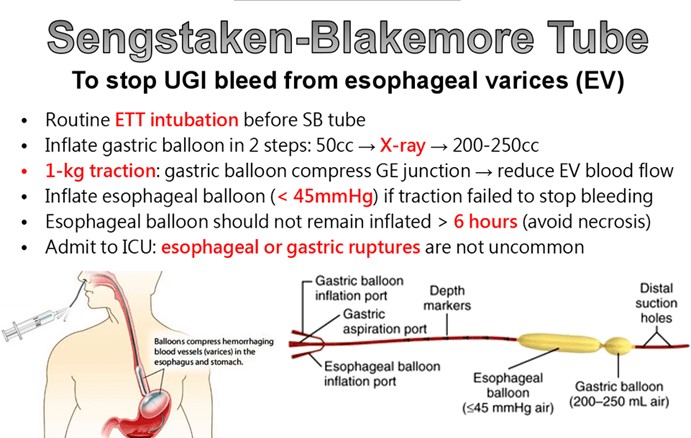
A nurse is caring for a client who has bleeding esophageal varices and is being treated with a Sengstaken-Blakemore tube. Which of the following actions should the nurse perform?
Deflate the balloons for 5 min every 2 hr to prevent tissue necrosis.
Keep the head of the bed flat at all times to prevent the development of shock.
Maintain constant observation while the balloons are inflated.
Suction the tube every 2 hr and as needed to maintain patency.
The Correct Answer is C
Choice A Reason: This is incorrect. The balloons should not be deflated without a physician's order, as this can cause rebleeding or aspiration.
Choice B Reason: This is incorrect. The head of the bed should be elevated to 30 to 45 degrees to reduce pressure on the balloons and prevent gastric reflux.
Choice C Reason: This is correct. The nurse should monitor the client closely for signs of complications, such as airway obstruction, aspiration, or balloon rupture. The nurse should also keep scissors at the bedside to cut the tube and release the balloons in case of an emergency.
Choice D Reason: This is incorrect. The tube should not be suctioned, as this can damage the mucosa and cause bleeding. The nurse should only aspirate gastric contents through the gastric lumen to decompress the stomach.
Nursing Test Bank
Naxlex Comprehensive Predictor Exams
Related Questions
Correct Answer is A
Explanation
Choice A: Cold and numb sensation distal to the fistula site is a possible indication of venous insufficiency. Venous insufficiency is a condition in which the veins have difficulty returning blood from the limbs to the heart, resulting in blood pooling and reduced perfusion. A new arteriovenous fistula can cause increased blood flow through the artery and decreased blood flow through the vein, leading to venous insufficiency. This can manifest as coldness, numbness, tingling, or cyanosis in the fingers or hand below the fistula site.
Choice B: A raised red rash around the fistula site is not a possible indication of venous insufficiency. A raised red rash around the fistula site can indicate an allergic reaction, an infection, or an inflammation of the skin or subcutaneous tissue. The nurse should assess the rash for size, shape, color, texture, temperature, and drainage, and report any signs of infection or inflammation, such as fever, pus, or swelling.
Choice C: Pain in the right arm proximal to the fistula site is not a possible indication of venous insufficiency. Pain in the right arm proximal to the fistula site can indicate arterial insufficiency, which is a condition in which the arteries have difficulty delivering oxygen-rich blood to the tissues, resulting in ischemia and necrosis. Arterial insufficiency can be caused by atherosclerosis, thrombosis, embolism, or vasospasm. The nurse should assess the pain for location, intensity, duration, frequency, and quality, and report any signs of ischemia or necrosis, such as pallor, coolness, weak pulses, or ulceration.
Choice D: Foul-smelling drainage from the fistula site is not a possible indication of venous insufficiency. Foul-smelling drainage from the fistula site can indicate an infection of the fistula or surrounding tissue. The nurse should assess the drainage for color, odor, amount, and consistency, and report any signs of infection or sepsis, such as fever, chills, malaise, or hypotension.
Correct Answer is B
Explanation
Choice A: Ask the client to shrug his shoulders against passive resistance is not an assessment that will give the nurse information about the function of cranial nerve III. This assessment will test the function of cranial nerve XI, which is the accessory nerve. The accessory nerve innervates the trapezius and sternocleidomastoid muscles, which are involved in shoulder and neck movements.
Choice B: Instruct the client to look up and down without moving his head is an assessment that will give the nurse information about the function of cranial nerve III. Cranial nerve III is the oculomotor nerve, which innervates four of the six extraocular muscles that control eye movements. The oculomotor nerve also controls pupil size and lens shape. By instructing the client to look up and down without moving his head, the nurse can assess the ability of the oculomotor nerve to move the eyes vertically and adjust to different distances.
Choice C: Observe the client's ability to smile and frown is not an assessment that will give the nurse information about the function of cranial nerve III. This assessment will test the function of cranial nerve VII, which is the facial nerve. The facial nerve innervates the muscles of facial expression, which are involved in smiling, frowning, blinking, and other facial movements.
Choice D: Have the client stand with his eyes closed and touch his nose is not an assessment that will give the nurse information about the function of cranial nerve III. This assessment will test the function of cranial nerve VIII, which is the vestibulocochlear nerve. The vestibulocochlear nerve innervates the inner ear and is responsible for hearing and balance. By having the client stand with his eyes closed and touch his nose, the nurse can assess the ability of the vestibulocochlear nerve to maintain equilibrium and coordination.
Whether you are a student looking to ace your exams or a practicing nurse seeking to enhance your expertise , our nursing education contents will empower you with the confidence and competence to make a difference in the lives of patients and become a respected leader in the healthcare field.
Visit Naxlex, invest in your future and unlock endless possibilities with our unparalleled nursing education contents today
Report Wrong Answer on the Current Question
Do you disagree with the answer? If yes, what is your expected answer? Explain.
Kindly be descriptive with the issue you are facing.
