A nurse is assessing a full-term newborn. Which of the following findings should the nurse report to the provider?
Respiratory rate 55/min
Blood pressure 80/50 mm Hg
Temperature 36.5°C (97.7°F)
Heart rate 72/min
The Correct Answer is D
Heart rate is one of the vital signs that reflects the health and well-being of a newborn. It is measured by counting the number of heart beats per minute, either by listening to the chest with a stethoscope or by feeling the pulse at the wrist, elbow, or groin. Heart rate can vary depending on the newborn's activity level, temperature, and emotional state¹.
The normal range for heart rate in full-term newborns is 120 to 160 beats per minute. The heart rate may be slightly higher or lower depending on the newborn's age, weight, and gestational age. For example, premature newborns may have a higher heart rate than term newborns, and heavier newborns may have a lower heart rate than lighter newborns¹².
A heart rate that is too high (tachycardia) or too low (bradycardia) can indicate a problem with the newborn's heart function, oxygenation, or circulation. Some of the possible causes of abnormal heart rate in newborns are:
- Congenital heart defects: structural abnormalities of the heart that are present at birth and affect the blood flow through the heart and the body. They can cause cyanosis (bluish skin color), murmur (abnormal heart sound), poor feeding, or failure to thrive¹³.
- Arrhythmias: irregular or abnormal heart rhythms that can affect the electrical impulses that control the heartbeat. They can cause palpitations (feeling of skipped or extra beats), dizziness, fainting, or cardiac arrest¹³.
- Hypoxia: lack of oxygen in the blood or tissues that can affect the brain and other organs. It can be caused by respiratory distress, anemia, infection, or birth asphyxia. It can cause bradycardia, apnea (pauses in breathing), seizures, or coma¹⁴.
- Hypothermia: low body temperature that can affect the metabolism and organ function. It can be caused by exposure to cold environment, infection, or prematurity. It can cause bradycardia, lethargy, poor feeding, or hypoglycemia (low blood sugar)¹⁴.
- Sepsis: severe infection that can affect the whole body and cause inflammation and organ damage. It can be caused by bacteria, viruses, fungi, or parasites that enter the bloodstream from the mother, the umbilical cord, or the environment. It can cause tachycardia, fever, chills, poor feeding, or shock¹⁴.
Therefore, the nurse should report a heart rate of 72/min to the provider as an abnormal finding and monitor the newborn for any other signs of distress or illness. The provider may order further tests or treatments to determine the cause and severity of the low heart rate and prevent any complications.
The other findings are not findings that the nurse should report to the provider because they are within the
normal range for full-term newborns:
- a) Respiratory rate 55/min is within the normal range for respiratory rate in full-term newborns. The normal range for respiratory rate in full-term newborns is 40 to 60 breaths per minute. The respiratory rate may vary depending on the newborn's activity level, temperature and emotional state¹².
- b) Blood pressure 80/50 mm Hg is within the normal range for blood pressure in full-term newborns. The normal range for blood pressure in full-term newborns is 65 to 95 mm Hg for systolic pressure (the top number) and 30 to 60 mm Hg for diastolic pressure (the bottom number). The blood pressure may vary depending on the newborn's age, weight, and gestational age¹².
- c) Temperature 36.5°C (97.7°F) is within the normal range for temperature in full-term newborns. The normal range for temperature in full-term newborns is 36.5°C to 37.5°C (97.7°F to 99.5°F). The temperature may vary depending on the newborn's activity level, clothing, and environment¹².
Nursing Test Bank
Naxlex Comprehensive Predictor Exams
Related Questions
Correct Answer is D
Explanation
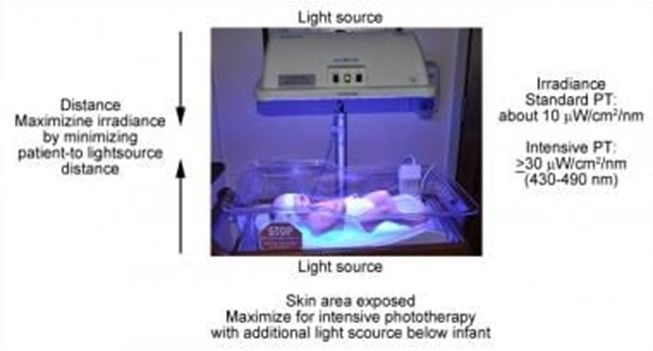
Phototherapy is a treatment that uses light to lower the level of bilirubin in the blood of newborns who have jaundice. Jaundice is a condition that causes yellowing of the skin and eyes due to high levels of bilirubin, a waste product that is normally removed by the liver. Phototherapy helps the body break down and eliminate bilirubin through urine and stool¹.
Phototherapy can be done at home or in the hospital, depending on the severity of jaundice and the type of light used. The most common types of light are fluorescent lamps, halogen lamps, or light-emitting diodes (LEDs). The light can be delivered through overhead units, fiber-optic blankets, or fiber-optic pads. The light should cover as much of the newborn's skin as possible, except for the eyes and genitals¹².
The nurse should follow certain guidelines when caring for a newborn who is receiving phototherapy, such
as:
- Monitor the newborn's temperature, hydration, weight, and urine and stool output regularly
- Protect the newborn's eyes with eye patches or goggles to prevent eye damage
- Turn the newborn every 2 to 4 hours to expose different parts of the body to the light
- Feed the newborn frequently to prevent dehydration and promote bilirubin excretion
- Check the newborn's skin color and bilirubin level periodically to evaluate the effectiveness of
phototherapy
- Provide emotional support and education to the parents about jaundice and phototherapy
One of the important guidelines is to avoid using lotion or ointment on the newborn's skin during phototherapy. This is because lotion or ointment can block the light from reaching the skin and reduce the effectiveness of phototherapy. Lotion or ointment can also cause skin irritation, rash, or burns if they react with the light. The newborn's skin should be clean and dry before phototherapy¹²³.
The other options are not actions that the nurse should include in the plan of care:
- a) Keep the newborn supine throughout treatment. This is not correct because keeping the newborn in one position can limit the exposure of different parts of the body to the light and reduce the effectiveness of phototherapy. The nurse should turn the newborn every 2 to 4 hours to expose different parts of the body to the light¹².
- b) Dress the newborn in lightweight clothing. This is not correct because dressing the newborn in clothing can block the light from reaching the skin and reduce the effectiveness of phototherapy. The newborn should be undressed except for a diaper during phototherapy¹².
- c) Measure the newborn's temperature every 8 hours. This is not correct because measuring the newborn's temperature every 8 hours may not be frequent enough to detect any changes in temperature that may occur during phototherapy. Phototherapy can cause overheating or hypothermia in newborns, depending on the type and intensity of light used. The nurse should monitor the newborn's temperature more often, such as every 2 to 4 hours, and adjust the room temperature or use blankets as needed¹².
Correct Answer is A
Explanation
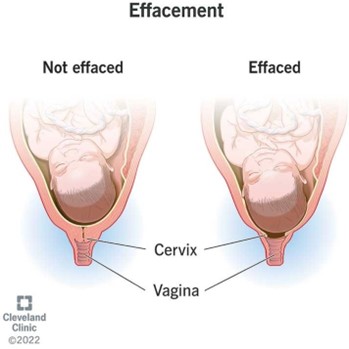
A spontaneous abortion (also called a miscarriage) is the unexpected ending of a pregnancy in the first 20 weeks of gestation. The major symptoms of a spontaneous abortion are abdominal cramps and bleeding from the vagina, sometimes with clots and/or bits of tissue³. A dilated cervix indicates that abortion is inevitable¹. Other symptoms may include low back ache, a decrease in pregnancy symptoms, and leaking amniotic fluid.
The other options are not answers because they are not indicative of an imminent spontaneous abortion.
b. Slight abdominal cramps
Slight abdominal cramps are a common symptom of early pregnancy and do not necessarily mean that a miscarriage is happening. However, if the cramps are severe, persistent, or accompanied by bleeding, then they could be a sign of a problem and should be reported to the provider.
c. Elevated hCG
hCG (human chorionic gonadotropin) is a hormone produced by the placenta during pregnancy. It can be measured in the blood or urine to confirm pregnancy or monitor its progress. Elevated hCG levels are not a sign of a spontaneous abortion, but rather a normal finding in early pregnancy. In fact, low or decreasing hCG levels may indicate a miscarriage or an ectopic pregnancy.
d. Scant bright red spotting
Scant bright red spotting is another common symptom of early pregnancy and does not necessarily mean that a miscarriage is happening. It may be caused by implantation bleeding, cervical irritation, or sexual intercourse. However, if the spotting is heavy, dark, or accompanied by cramps or pain, then it could be a sign of a problem and should be reported to the provider.
Whether you are a student looking to ace your exams or a practicing nurse seeking to enhance your expertise , our nursing education contents will empower you with the confidence and competence to make a difference in the lives of patients and become a respected leader in the healthcare field.
Visit Naxlex, invest in your future and unlock endless possibilities with our unparalleled nursing education contents today
Report Wrong Answer on the Current Question
Do you disagree with the answer? If yes, what is your expected answer? Explain.
Kindly be descriptive with the issue you are facing.
