A nurse is assessing a child who has bacterial pneumonia.
Which of the following manifestations should the nurse expect?
Drooling
Tinnitus
Malaise
Rhinorrhea
The Correct Answer is C
The correct answer is choice C, malaise.
Malaise is a general feeling of discomfort, weakness, or illness that can be a sign of infection. According to the health search result from Focus Medica , bacterial pneumonia is an infection of the air sacs in one or both lungs that causes symptoms such as cough with phlegm, fever, chills, and difficulty breathing.
Malaise is one of the symptoms that may follow these signs of infection.
Choice A, drooling, is wrong because it is not a typical symptom of bacterial pneumonia.
Drooling can be caused by other conditions, such as sore throat, dental problems, or neurological disorders.
Choice B, tinnitus, is wrong because it is not a symptom of bacterial pneumonia either.
Tinnitus is a ringing or buzzing sound in the ears that can be caused by exposure to loud noise, ear infections, or other ear problems.
Choice D, rhinorrhea, is wrong because it is not specific to bacterial pneumonia.
Rhinorrhea is a runny nose that can be caused by many factors, such as allergies, colds, or sinus infections.
Rhinorrhea can sometimes occur with viral pneumonia, but not usually with bacterial pneumonia.
Nursing Test Bank
Naxlex Comprehensive Predictor Exams
Related Questions
Correct Answer is A
Explanation
Choice A reason:
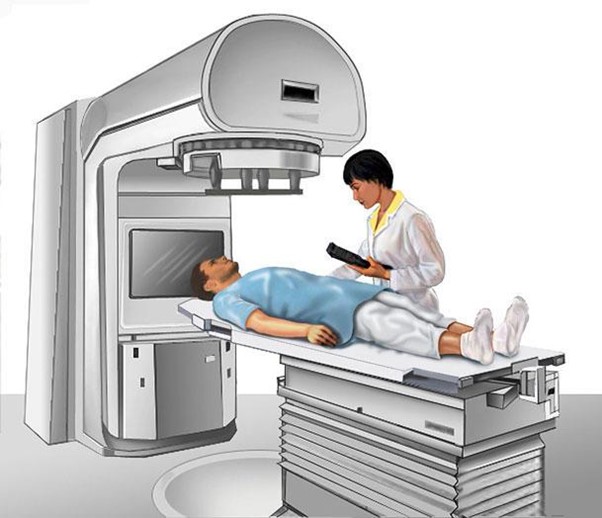
"You might experience altered taste sensations" is the correct statement. When providing teaching to a client about to undergo external radiation therapy for cancer, the nurse should include information about potential side effects and what to expect during the treatment. One common side effect of radiation therapy, especially when the treatment is focused on or near the head and neck region, is altered taste sensations. Radiation can affect the taste buds and lead to changes in how foods taste.
Choice B reason:
"Use rubbing alcohol to remove the ink markings. “The statement is incorrect. The ink markings made on the client's skin are used as reference points for the radiation therapy treatment. It is essential not to remove these markings, as they are crucial for accurate positioning during each treatment session. The nurse should instruct the client not to tamper with the markings, and the radiation therapy team will remove them when they are no longer needed.
Choice C reason:
"Wear a binder over the radiation site." The statement is incorrect. Wearing a binder over the radiation site is not a standard practice during external radiation therapy. The client should be instructed to follow the specific guidelines provided by the radiation therapy team regarding clothing and positioning during treatments. The use of binders or other tight clothing over the treatment area may not be recommended, as it can cause discomfort or interfere with the delivery of radiation.
Choice D reason
"Wash your skin thoroughly with a washcloth after each treatment." Is incorrect statement. During radiation therapy, the skin in the treatment area can become sensitive. It is essential for the client to follow the specific instructions provided by the radiation therapy team regarding skin care. Generally, the client should avoid using harsh soaps or scrubbing the skin vigorously. Instead, they should gently cleanse the area with a mild soap or as directed by their healthcare providers.
Correct Answer is C
Explanation
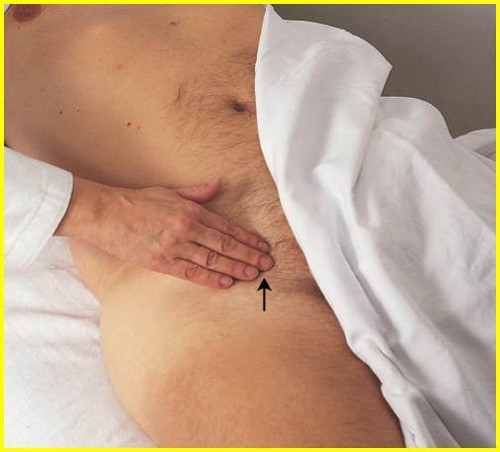
This is because coarctation of the aorta is a congenital condition where the aorta is narrow, usually in the area where the ductus arteriosus inserts. This causes a decrease in blood flow to the lower body, resulting in weak or absent pulses in the femoral arteries.
The other choices are incorrect for the following reasons:
- Choice A, frequent nosebleeds, is not a typical sign of coarctation of the aorta.
Nosebleeds can be caused by many factors, such as dry air, allergies, trauma, or bleeding disorders.
- Choice B, upper extremity hypotension, is also not a common finding in coarctation of the aorta. In fact, patients with this condition may have high blood pressure in the upper extremities due to the increased resistance of the narrowed aorta.
- Choice D, increased intracranial pressure, is not directly related to coarctation of the aorta.
Increased intracranial pressure can be caused by various conditions that affect the brain, such as head injury, stroke, infection, or tumor.
Normal ranges for blood pressure and pulse vary depending on age, sex, and health status.
However, some general guidelines are:
- Blood pressure: less than 120/80 mmHg for adults; less than 95/65 mmHg for infants.
- Pulse: 60 to 100 beats per minute for adults; 100 to 160 beats per minute for infants.
Whether you are a student looking to ace your exams or a practicing nurse seeking to enhance your expertise , our nursing education contents will empower you with the confidence and competence to make a difference in the lives of patients and become a respected leader in the healthcare field.
Visit Naxlex, invest in your future and unlock endless possibilities with our unparalleled nursing education contents today
Report Wrong Answer on the Current Question
Do you disagree with the answer? If yes, what is your expected answer? Explain.
Kindly be descriptive with the issue you are facing.
