A nurse in the emergency department is caring for a client who has an epidural hematoma following a motor-vehicle crash. Which of the following is an expected finding for this client?
Drainage of clear fluid from the ears
Alternating periods of alertness and unconsciousness
Narrowing pulse pressure
Extensive bruising in the mastoid area
The Correct Answer is B
Choice A: Drainage of clear fluid from the ears is not an expected finding for a client who has an epidural hematoma, but rather a sign of a basilar skull fracture, which is a different type of head injury. The clear fluid is cerebrospinal fluid (CSF), which leaks from the brain through the fractured skull.
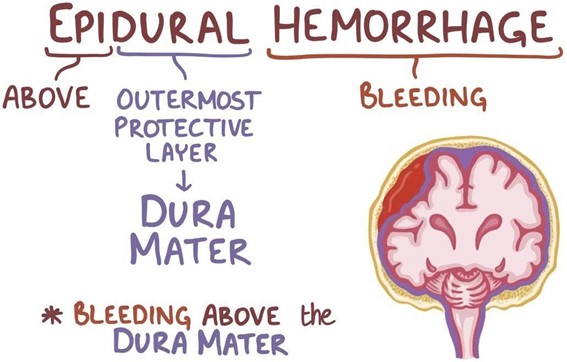
Choice B: Alternating periods of alertness and unconsciousness is an expected finding for a client who has an epidural hematoma, because it indicates a rapid increase in intracranial pressure (ICP) due to bleeding between the dura mater and the skull. The client may have a brief loss of consciousness at the time of injury, followed by a lucid interval, and then a rapid deterioration of mental status.
Choice C: Narrowing pulse pressure is not an expected finding for a client who has an epidural hematoma, but rather a sign of increased ICP due to any cause. Pulse pressure is the difference between systolic and diastolic blood pressure. As ICP rises, it compresses the brainstem and causes bradycardia and hypertension, resulting in a decreased pulse pressure.
Choice D: Extensive bruising in the mastoid area is not an expected finding for a client who has an epidural hematoma, but rather a sign of a basilar skull fracture, which is a different type of head injury. The bruising is also known as Batle's sign, and it occurs due to blood pooling behind the ear.
Nursing Test Bank
Naxlex Comprehensive Predictor Exams
Related Questions
Correct Answer is B
Explanation
Choice A Reason: This is incorrect because the client is not in deep coma, as the Glasgow Coma Scale (GCS) score ranges from 3 to 15, with 3 being the lowest possible score and indicating deep coma or death.
Choice B Reason: This is correct because the client needs total nursing care, as the GCS score of 6 indicates a severe brain injury and a very low level of consciousness. The client may only open his eyes to pain, make incomprehensible sounds, and have abnormal flexion to pain.
Choice C Reason: This is incorrect because the client is not alert and oriented, as the GCS score of 6 indicates a severe brain injury and a very low level of consciousness. The client may not be able to follow commands, answer questions, or recognize people or places.
Choice D Reason: This is incorrect because the client is not responding to verbal stimuli, as the GCS score of 6 indicates a severe brain injury and a very low level of consciousness. The client may only respond to painful stimuli, such as pinching or squeezing.

Correct Answer is A
Explanation
The correct answer is a. Respiratory status.
Choice A: Respiratory Status
Reason: After the evacuation of a subdural hematoma, monitoring the respiratory status is crucial. This is because changes in respiratory patterns can indicate increased intracranial pressure (ICP) or brainstem compression, which are life-threatening conditions. Ensuring that the airway is clear and that the patient is breathing adequately is the top priority. Normal respiratory rate for adults is 12-20 breaths per minute.
Choice B: Temperature
Reason: While monitoring temperature is important to detect infections or other complications, it is not the immediate priority in the acute postoperative period following a subdural hematoma evacuation. Fever can indicate infection, but it is less likely to cause immediate life-threatening complications compared to respiratory issues.
Choice C: Intracranial Pressure
Reason: Monitoring intracranial pressure (ICP) is very important in patients with brain injuries. Normal ICP ranges from 5-15 mmHg. However, changes in respiratory status can be an early indicator of increased ICP. Therefore, while ICP monitoring is critical, ensuring the patient’s respiratory status is stable takes precedence.
Choice D: Serum Electrolytes
Reason: Serum electrolytes are important to monitor for overall metabolic stability and to detect imbalances that could affect neurological function. Normal ranges for key electrolytes are: Sodium (135-145 mEq/L), Potassium (3.5-4.5 mEq/L), and Chloride (80-100 mEq/L). However, these are not the immediate priority in the acute phase following surgery compared to respiratory status.
Whether you are a student looking to ace your exams or a practicing nurse seeking to enhance your expertise , our nursing education contents will empower you with the confidence and competence to make a difference in the lives of patients and become a respected leader in the healthcare field.
Visit Naxlex, invest in your future and unlock endless possibilities with our unparalleled nursing education contents today
Report Wrong Answer on the Current Question
Do you disagree with the answer? If yes, what is your expected answer? Explain.
Kindly be descriptive with the issue you are facing.
