A client with diabetes mellitus is being admitted to the hospital for surgery. The client has been taking Glucocorticoids (Prednisone) long-term for uncontrolled COPD. Which of the following must the nurse consider when she is obtaining a health history? (Select All that Apply.)
Due to the use of long-term glucocorticoids her medication must not be abruptly discontinued to avoid adrenal suppression
The client may develop low blood pressure
The use of long-term glucocorticoids places the client at risk for increased susceptibility to infection
The use of long-term glucocorticoids may have contributed to a spike in blood glucose levels
The client will most likely experience more pain
Correct Answer : A,C,D
The nurse must consider the following when obtaining a health history for a client with diabetes mellitus who has been taking glucocorticoids (prednisone) long-term for uncontrolled COPD:
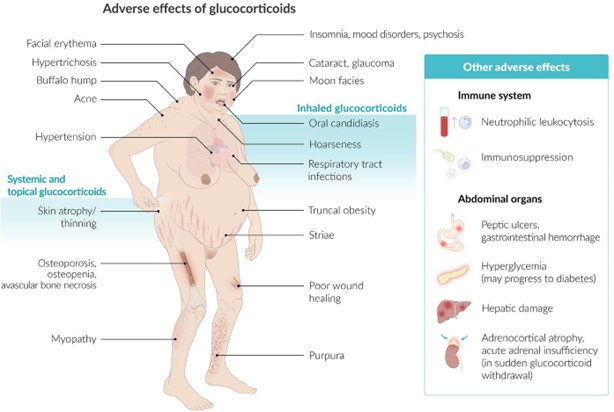
- Due to the use of long-term glucocorticoids, the medication must not be abruptly discontinued to avoid adrenal suppression. Abruptly stopping glucocorticoids can lead to adrenal insufficiency and a potentially life-threatening condition. Gradual tapering of the medication is necessary under medical supervision.
- The use of long-term glucocorticoids may contribute to a spike in blood glucose levels. Glucocorticoids can cause insulin resistance and increase blood sugar levels, which can be problematic for individuals with diabetes mellitus.
- The use of long-term glucocorticoids places the client at risk for increased susceptibility to infection. Glucocorticoids can suppress the immune system, making the client more susceptible to infections. This is important to consider, especially in a hospital setting where the risk of acquiring infections may be higher.
Regarding the other options:
The client may develop low blood pressure: While glucocorticoids can cause fluid retention and increased blood pressure, they are not typically associated with low blood pressure.
The client will most likely experience more pain: The use of glucocorticoids is not directly related to increased pain perception. Pain management may be influenced by various factors, but it is not specifically attributed to long-term glucocorticoid use.
Nursing Test Bank
Naxlex Comprehensive Predictor Exams
Related Questions
Correct Answer is C
Explanation
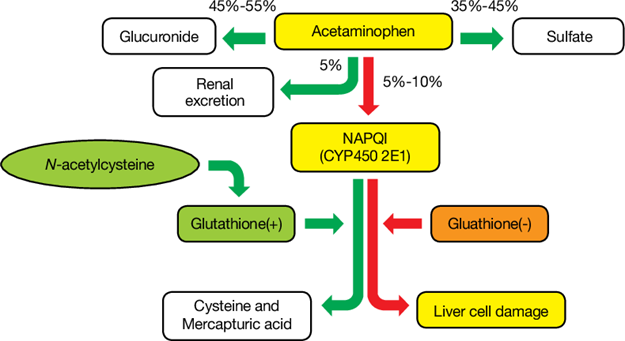
Acetaminophen overdose can cause liver damage, and acetylcysteine is used as an antidote to prevent or minimize the liver injury caused by acetaminophen toxicity. Acetylcysteine works by replenishing glutathione, a substance that helps neutralize the toxic byproducts of acetaminophen metabolism in the liver.
It is important to note that acetylcysteine is specifically indicated for acetaminophen overdose and may not be effective or appropriate for overdosage of other drugs, such as ibuprofen, diphenhydramine, or amoxicillin.
Correct Answer is ["10"]
Explanation
To determine the mL of diphenhydramine elixir to administer per dose, we need to calculate the dose based on the prescribed amount and the concentration of the elixir.
Given:
Prescribed dose: 25 mg Concentration of elixir: 12.5 mg/5 mL
We can set up a proportion to find the equivalent mL for the prescribed dose: 25 mg / x mL = 12.5 mg / 5 mL
Cross-multiplying and solving for x, we get:
25 mg * 5 mL = 12.5 mg * x mL 125 mg = 12.5 mg * x mL
125 mg / 12.5 mg = x mL 10 mL = x mL
Therefore, the nurse should administer 10 mL of diphenhydramine elixir per dose.
Whether you are a student looking to ace your exams or a practicing nurse seeking to enhance your expertise , our nursing education contents will empower you with the confidence and competence to make a difference in the lives of patients and become a respected leader in the healthcare field.
Visit Naxlex, invest in your future and unlock endless possibilities with our unparalleled nursing education contents today
Report Wrong Answer on the Current Question
Do you disagree with the answer? If yes, what is your expected answer? Explain.
Kindly be descriptive with the issue you are facing.
