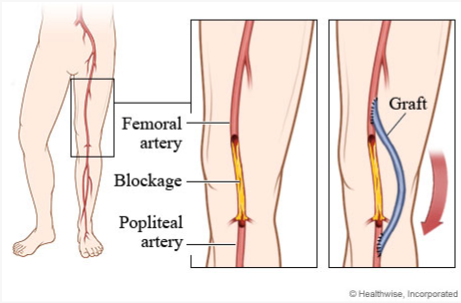
A client who has undergone a femoral to popliteal bypass graft surgery returns to the surgical unit. Which assessments should the nurse perform during the first postoperative day?
Assess pulse of affected extremity every 15 minutes at first.
Palpate the affected leg for pain during every assessment
Assess the client for signs and symptoms of compartment syndrome every 2 hours.
Perform Doppler evaluation once daily.
Correct Answer : A,B,C,D
Assess pulse of the affected extremity every 15 minutes at first: Frequent assessment of the pulse in the affected extremity is important to monitor for any changes in blood flow. This allows the nurse to identify any potential complications such as graft occlusion or compromised circulation promptly.
Palpate the affected leg for pain during every assessment: Assessing for pain in the affected leg is crucial to identify any signs of ischemia or inadequate perfusion. Increased pain could indicate reduced blood flow or other complications that require immediate attention.
Assess the client for signs and symptoms of compartment syndrome every 2 hours: Compartment syndrome can occur after vascular surgeries, and early recognition is vital. The nurse should assess for signs and symptoms such as pain, numbness, tingling, increased swelling, and tense compartments. Regular assessment every 2 hours can help detect compartment syndrome promptly and prevent further complications.
Perform Doppler evaluation once daily: Doppler evaluation may be ordered by the healthcare provider to assess blood flow and graft patency. However, the frequency of Doppler evaluation may vary depending on the client's condition and the healthcare provider's orders. Once daily assessment is not sufficient if there are concerns regarding blood flow or graft viability.
Nursing Test Bank
Naxlex Comprehensive Predictor Exams
Related Questions
Correct Answer is D
Explanation
An ABI of 0.89 indicates a reduced blood flow to the lower extremities, which is suggestive of peripheral arterial disease (PAD). In PAD, there is narrowing or blockage of the arteries that supply blood to the legs and feet. Medications like clopidogrel and simvastatin are commonly prescribed for individuals with PAD to manage the condition and reduce the risk of complications.
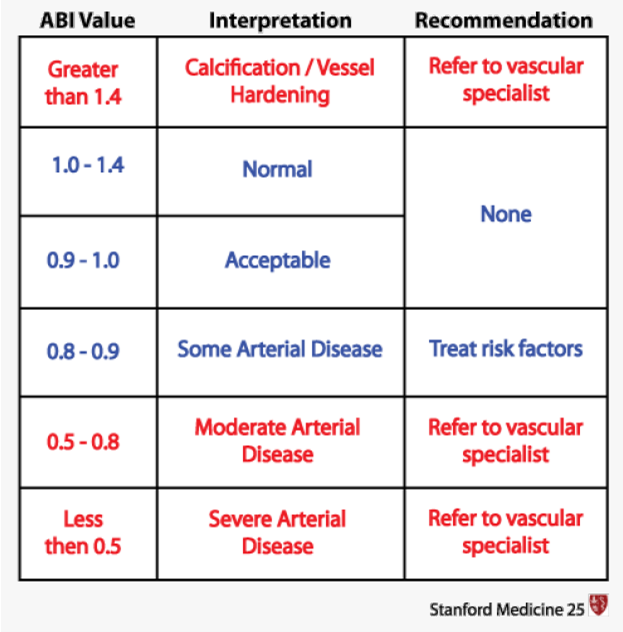
Here's an explanation of why the other options are not the most appropriate interventions:
Document the information as a normal finding: An ABI of 0.89 is not considered a normal finding. An ABI value below 0.9 is generally indicative of PAD or reduced blood flow to the lower extremities.
Prepare the client for an arterial bypass: An ABI value of 0.89 alone does not warrant immediate preparation for an arterial bypass. Arterial bypass surgery is typically considered for severe cases of PAD with significant symptoms that significantly impact the client's quality of life and other conservative treatments have not been successful.
Educate the client about the use of compression stockings: While compression stockings may be a part of the overall management of PAD, the ABI result alone does not indicate an immediate need for education about compression stockings. Other interventions, such as medication management, lifestyle modifications, and possibly revascularization procedures, may be more appropriate based on the severity of the PAD.
Correct Answer is D
Explanation
Helping to position a client for a portable x-ray generally involves physically assisting the client in moving into the appropriate position or adjusting their body as needed. This task can be safely delegated to the UAP as long as they have received proper training on how to safely assist with positioning and have a clear understanding of the specific instructions provided by the radiology department.
Assisting the client to take the beta-blocker involves administering medication, which falls within the scope of nursing practice and requires the nurse's expertise in medication administration and monitoring the client's response.
Transporting the client to the intensive care unit via a stretcher involves moving the client to another unit and may require additional monitoring and coordination of care during the transfer. This task is best performed by the nurse, who can assess the client's stability, ensure appropriate documentation, and communicate effectively with the receiving unit.
Providing discharge-teaching instructions to the client going home requires the nurse to provide information about medications, wound care, follow-up appointments, and other important instructions. This task involves comprehensive education and assessment ofthe client's understanding, and is best performed by the nurse to ensure accurate and complete information is provided.
Whether you are a student looking to ace your exams or a practicing nurse seeking to enhance your expertise , our nursing education contents will empower you with the confidence and competence to make a difference in the lives of patients and become a respected leader in the healthcare field.
Visit Naxlex, invest in your future and unlock endless possibilities with our unparalleled nursing education contents today
Report Wrong Answer on the Current Question
Do you disagree with the answer? If yes, what is your expected answer? Explain.
Kindly be descriptive with the issue you are facing.
