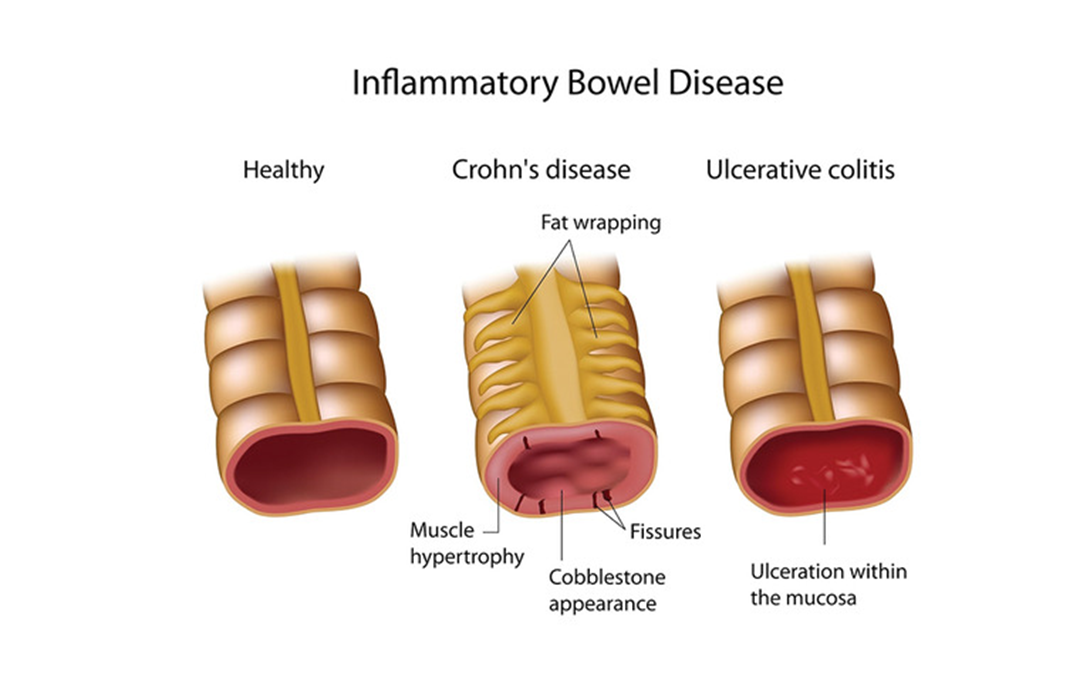
A client is hospitalized with an inflammatory bowel disease (IBD) exacerbation and is being treated with a corticosteroid. The client develops a rigid abdomen with rebound tenderness. Which action should the nurse take?
Measure capillary glucose level.
Encourage ambulation in the room.
Monitor for bloody diarrheal stools.
Obtain vital sign measurements.
The Correct Answer is D
Choice A reason: Measuring capillary glucose level is not a priority action for a client with a rigid abdomen and rebound tenderness. These signs indicate peritonitis, which is a serious complication of IBD that requires immediate attention. Corticosteroids can increase blood glucose levels, but this is not an urgent concern in this situation.
Choice B reason: Encouraging ambulation in the room is not appropriate for a client with a rigid abdomen and rebound tenderness. These signs indicate peritonitis, which is a serious complication of IBD that requires immediate attention. Ambulation can worsen the pain and inflammation, and increase the risk of bowel perforation.
Choice C reason: Monitoring for bloody diarrheal stools is important for a client with IBD, but not a priority action for a client with a rigid abdomen and rebound tenderness. These signs indicate peritonitis, which is a serious complication of IBD that requires immediate attention. Bloody stools can be a sign of ulceration or bleeding in the bowel, but they are not specific to peritonitis.
Choice D reason: Obtaining vital sign measurements is the priority action for a client with a rigid abdomen and rebound tenderness. These signs indicate peritonitis, which is a serious complication of IBD that requires immediate attention. Vital signs can reveal signs of infection, inflammation, shock, and organ failure, which can guide the appropriate interventions and treatments.
Nursing Test Bank
Naxlex Comprehensive Predictor Exams
Related Questions
Correct Answer is B
Explanation
Choice A reason: This is incorrect because hepatorenal failure is a condition that involves both liver and kidney dysfunction, usually as a complication of cirrhosis or portal hypertension. The symptoms of hepatorenal failure may include jaundice, ascites, edema, oliguria, or encephalopathy. However, these are not consistent with the client's presentation of fever, abdominal pain, vomiting, and elevated amylase and lipase levels.
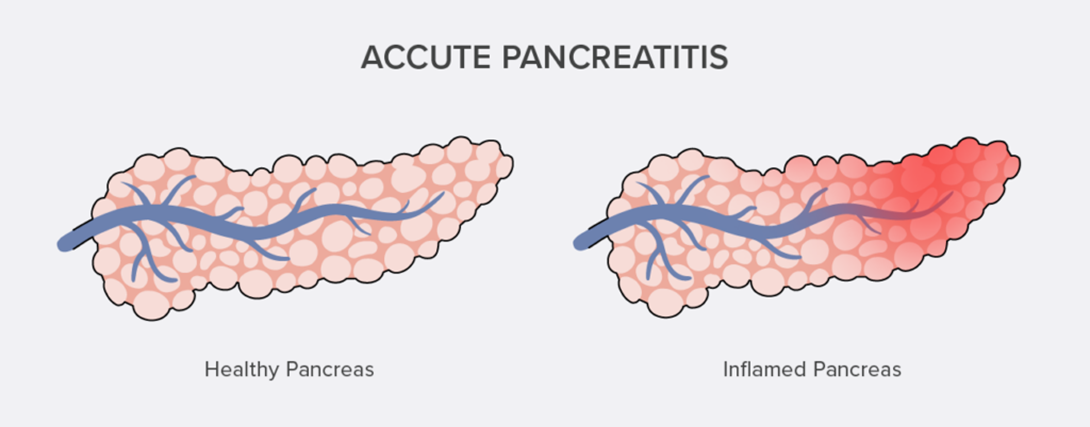
Choice B reason: This is correct because acute pancreatitis is an inflammation of the pancreas that can be caused by gallstones, alcohol abuse, trauma, infection, or drugs. The symptoms of acute pancreatitis may include fever, upper abdominal pain that radiates to the back, nausea, vomiting, and elevated amylase and lipase levels. These are consistent with the client's presentation and suggest that the cholecystectomy may have triggered an attack of acute pancreatitis.
Choice C reason: This is incorrect because surgical site infection is an infection that occurs at or near the incision site after surgery. The symptoms of surgical site infection may include redness, swelling, warmth, pus drainage, or pain at the wound site. However, these are not consistent with the client's presentation of fever, abdominal pain radiating to the back, vomiting, and elevated amylase and lipase levels.
Choice D reason: This is incorrect because biliary duct obstruction is a blockage of the bile ducts that carry bile from the liver and gallbladder to the intestine. The causes of biliary duct obstruction may include gallstones, tumors, inflammation, or scarring. The symptoms of biliary duct obstruction may include jaundice, dark urine, pale stools, itching, or abdominal pain. However, these are not consistent with the client's presentation of fever, abdominal pain radiating to the back, vomiting, and elevated amylase and lipase levels.
Correct Answer is C
Explanation
Choice A reason: Redness and edema noted at the incision site are signs of inflammation, which are normal in the early stages of wound healing. The nurse should monitor the site for signs of infection, such as purulent drainage, increased pain, or fever.
Choice B reason: Apical heart rate of 100 to 110 beats/minute is a sign of tachycardia, which may be caused by pain, anxiety, dehydration, or blood loss. The nurse should assess the client's vital signs, fluid status, and hemoglobin level, and administer pain medication as prescribed.
Choice C reason: High-pitched sound heard upon inspiration is a sign of stridor, which is a life-threatening emergency that indicates airway obstruction. The nurse should call for help, administer oxygen, and prepare for intubation or tracheostomy.
Choice D reason: Pain rating of 8 on a scale of 0 to 10 is a sign of severe pain, which may impair the client's recovery and increase the risk of complications. The nurse should administer pain medication as prescribed and use non-pharmacological methods to relieve pain, such as positioning, distraction, or relaxation techniques.
Whether you are a student looking to ace your exams or a practicing nurse seeking to enhance your expertise , our nursing education contents will empower you with the confidence and competence to make a difference in the lives of patients and become a respected leader in the healthcare field.
Visit Naxlex, invest in your future and unlock endless possibilities with our unparalleled nursing education contents today
Report Wrong Answer on the Current Question
Do you disagree with the answer? If yes, what is your expected answer? Explain.
Kindly be descriptive with the issue you are facing.
