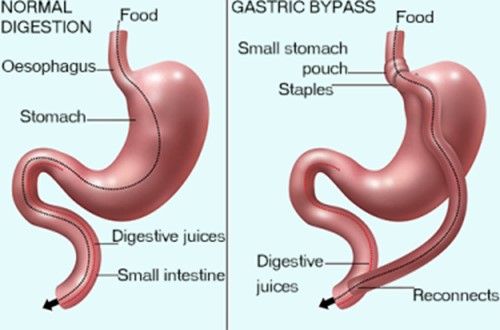
What discharge teaching will the nurse provide to a patient who has gastric bypass surgery? Select all that apply.
Each of your meals should contain about 10 tablespoons of food.
You are likely to have little urine output for the first few weeks.
Report any back, shoulder, or abdominal pain to the surgeon.
Be certain to stay hydrated by drinking water.
Solid food can be introduced back into the diet in a week.
Correct Answer : A,C,D
Each of your meals should contain about 10 tablespoons of food: After gastric bypass surgery, the stomach's size is reduced, and the patient's capacity to consume large quantities of food is limited. It is important to educate the patient about appropriate portion sizes to avoid overeating and potential complications.
Be certain to stay hydrated by drinking water: Hydration is crucial after gastric bypass surgery. Patients should be advised to drink enough water throughout the day to prevent dehydration and ensure proper bodily function.
Solid food can be introduced back into the diet in a week: Following gastric bypass surgery, the diet is initially limited to liquid and pureed foods. Gradually, solid foods can be reintroduced into the diet over time, typically after a week or as directed by the surgeon. This information is important for the patient to understand the progression of their diet post-surgery. You are likely to have little urine output for the first few weeks: This statement is not true and may cause unnecessary concern for the patient. Urine output should not be affected by gastric bypass surgery unless there are other complications.
Report any back, shoulder, or abdominal pain to the surgeon: While it is important to report any significant pain or discomfort to the surgeon, including back, shoulder, or abdominal pain, this is not specific to discharge teaching for gastric bypass surgery. Pain management and reporting should be covered during the post-operative care instructions, but it is not limited to discharge teaching alone.
Nursing Test Bank
Naxlex Comprehensive Predictor Exams
Related Questions
Correct Answer is C
Explanation
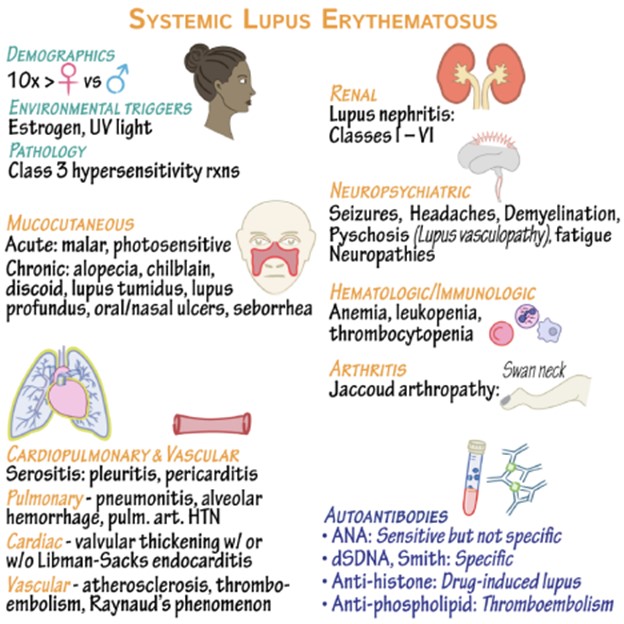
Excessive exposure to UV light, such as sunlight or tanning beds, is a known trigger for SLE exacerbations. It is important for individuals with SLE to protect their skin from the sun by wearing protective clothing, using sunscreen, and avoiding direct sunlight during peak hours. Having a family history of SLE increases the risk of developing the disease. While it is not a trigger in itself, it is an important piece of information for the client to be aware of, as it may indicate a genetic predisposition to the condition.
Acetaminophen is a commonly used over-the-counter pain reliever. While it can help manage pain associated with SLE, it is not typically considered a trigger for exacerbations. Menopause, which marks the end of a woman's reproductive years, does not directly trigger SLE exacerbations. However, hormonal changes during menopause can potentially affect disease activity in some individuals. It is important for the client to discuss any changes or concerns with their healthcare provider to manage their symptoms effectively.
Correct Answer is B
Explanation
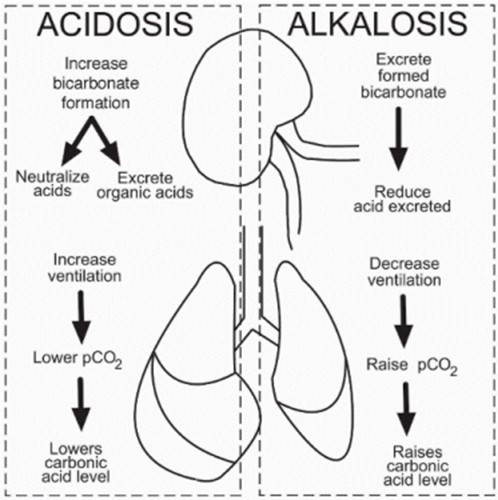
Respiratory acidosis is a primary acid-base imbalance that occurs when there is an excess of carbon dioxide (CO2) in the body due to impaired ventilation or inadequate removal of CO2 from the lungs. In this case, Colleen's depressed ventilation, indicated by shallow and slow respirations, can lead to inadequate elimination of CO2 from her body. The excessive CO2 levels can result in an accumulation of carbonic acid (H2CO3) in the blood, leading to an increase in acidity and a decrease in pH.
The profuse bleeding from both ears indicates a potential head injury, which can lead to decreased neurological function and impaired control over the respiratory center in the brain. This can further contribute to depressed ventilation and the development of respiratory acidosis. Metabolic acidosis, characterized by a decrease in bicarbonate (HCO3-) levels or an increase in non-carbonic acids in the blood, is not the primary acid-base imbalance in this case since the scenario does not provide information indicating a primary metabolic disorder. Respiratory alkalosis, characterized by decreased levels of CO2 in the blood, leading to increased pH and alkalinity, is not the primary acid-base imbalance in this case. The depressed ventilation and associated increase in CO2 levels indicate the opposite, respiratory acidosis. Metabolic alkalosis, characterized by an increase in bicarbonate levels or a decrease in non-carbonic acids, is not the primary acid-base imbalance in this case as the scenario does not provide information indicating a primary metabolic disorder.
Whether you are a student looking to ace your exams or a practicing nurse seeking to enhance your expertise , our nursing education contents will empower you with the confidence and competence to make a difference in the lives of patients and become a respected leader in the healthcare field.
Visit Naxlex, invest in your future and unlock endless possibilities with our unparalleled nursing education contents today
Report Wrong Answer on the Current Question
Do you disagree with the answer? If yes, what is your expected answer? Explain.
Kindly be descriptive with the issue you are facing.
