The practical nurse (PN) is assessing an older client with left-sided heart failure (HF). What intervention is most important for the PN to implement?
Inspect for sacral edema.
Measure urinary output.
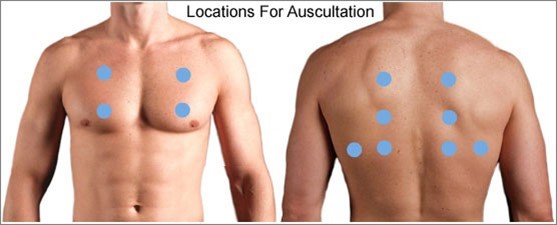
Auscultate all lung fields.
Check mental acuity.
The Correct Answer is C
When assessing an older client with left-sided heart failure (HF), the most important intervention for the practical nurse (PN) to implement is to auscultate all lung fields. Left-sided heart failure is characterized by the inability of the left ventricle to effectively pump blood, leading to fluid accumulation in the lungs. Auscultating all lung fields allows the PN to assess for the presence of abnormal lung sounds such as crackles, indicating pulmonary congestion.
Let's evaluate the other options:
a) Inspect for sacral edema.
Sacral edema is commonly associated with right-sided heart failure, not left-sided heart failure. While it is important to assess for edema in clients with heart failure, inspecting for sacral edema may not be the most immediate and crucial intervention in this specific case.
b) Measure urinary output.
Measuring urinary output is a valuable assessment in many clinical situations, but it may not be the most vital intervention in the context of left-sided heart failure. Monitoring urinary output is more relevant in assessing kidney function and fluid balance rather than directly assessing the severity of left-sided heart failure.
d) Check mental acuity.
Checking mental acuity is important in assessing the overall condition of the client, but it is not the most crucial intervention specifically related to left-sided heart failure. Mental status evaluation is more useful in identifying signs of altered mental status or potential complications, rather than directly assessing the impact of left-sided heart failure.
In summary, when assessing an older client with left-sided heart failure, the most important intervention for the practical nurse (PN) to implement is to auscultate all lung fields. This allows for the detection of abnormal lung sounds associated with pulmonary congestion, a hallmark sign of left-sided heart failure.
Nursing Test Bank
Naxlex Comprehensive Predictor Exams
Related Questions
Correct Answer is B
Explanation
Choice A rationale:
Serum blood glucose (BG) level is not directly related to the presence of purulent drainage at a burn wound site. Elevated BG levels might be seen in clients with diabetes or as a stress response, but they are not the primary indicator of infection or wound complications.
Choice C rationale:
Serum albumin levels can be relevant in assessing nutritional status and the body's ability to heal wounds. However, they do not directly indicate the presence of infection or purulent drainage. Low serum albumin levels may be seen in clients with malnutrition but do not provide immediate information about the wound.
Choice D rationale:
Hematocrit measures the percentage of red blood cells in the blood and is not directly related to the presence of purulent drainage at a burn wound site. Elevated hematocrit may indicate dehydration or hemoconcentration but does not specifically address the issue of wound infection.
Correct Answer is B
Explanation
Choice A rationale:
CP being one of the most common permanent physical disabilities in children is a general statement but does not directly address the mother's question about the progression of her child's impaired movements. It does not provide an explanation for the potential course of CP.
Choice B rationale:
Brain damage with CP is not progressive but does have a variable course. This response provides the best explanation to the mother's question. CP is a static neurological condition, which means that the initial brain injury that led to CP does not worsen over time. However, the functional abilities and impairments of a child with CP can vary widely and may change as the child grows and develops. Some children may improve with therapy and interventions, while others may have relatively stable impairments.
Choice C rationale:
Severe motor dysfunction determines the extent of successful habilitation is not entirely accurate. While the severity of motor dysfunction does play a role in the challenges a child with CP may face, it does not solely determine the extent of successful habilitation. Many factors, including early intervention, therapy, and individualized care, can influence a child's progress and potential for improvement.
Choice D rationale:
Continued development of the brain lesion determines the child's outcome is not an accurate statement. CP is primarily caused by non-pro
Whether you are a student looking to ace your exams or a practicing nurse seeking to enhance your expertise , our nursing education contents will empower you with the confidence and competence to make a difference in the lives of patients and become a respected leader in the healthcare field.
Visit Naxlex, invest in your future and unlock endless possibilities with our unparalleled nursing education contents today
Report Wrong Answer on the Current Question
Do you disagree with the answer? If yes, what is your expected answer? Explain.
Kindly be descriptive with the issue you are facing.
