A nurse is caring for a client who has atrial fibrillation and receives digoxin daily. Before administering this medication, which of the following actions should the nurse take?
Weigh the client.
Measure the client's blood pressure.
Measure the client's apical pulse.
Offer the client a light snack.
The Correct Answer is C
Choice A reason: Weighing the client is not a necessary action before administering digoxin, as it does not affect the dosage or effectiveness of the medication. Weighing the client may be important for monitoring fluid balance and edema, but it is not related to digoxin therapy.
Choice B reason: Measuring the client's blood pressure is not a necessary action before administering digoxin, as it does not affect the dosage or effectiveness of the medication. Digoxin is not a blood pressure-lowering medication, but a cardiac glycoside that increases the contractility and efficiency of the heart. Measuring the blood pressure may be important for monitoring hypertension, but it is not related to digoxin therapy.
Choice C reason: Measuring the client's apical pulse is a necessary action before administering digoxin, as it can help determine the safety and appropriateness of the medication. Digoxin can cause bradycardia (slow heart rate) as a side effect, which can be dangerous and symptomatic. The nurse should check the apical pulse for one full minute and withhold the medication if the pulse is below 60 beats per minute or above 100 beats per minute. The nurse should also report any abnormal or irregular rhythms to the provider.
Choice D reason: Offering the client a light snack is not a necessary action before administering digoxin, as it does not affect the absorption or effectiveness of the medication. Digoxin can be taken with or without food. Offering the client a light snack may be important for maintaining nutrition and hydration, but it is not related to digoxin therapy.
Nursing Test Bank
Naxlex Comprehensive Predictor Exams
Related Questions
Correct Answer is C
Explanation
Choice A reason: Vitamin K is the antidote for warfarin, not heparin. Vitamin K reverses the effects of warfarin by increasing the synthesis of clotting factors in the liver.
Choice B reason: Glucagon is the antidote for insulin, not heparin. Glucagon increases the blood glucose level by stimulating the breakdown of glycogen in the liver.
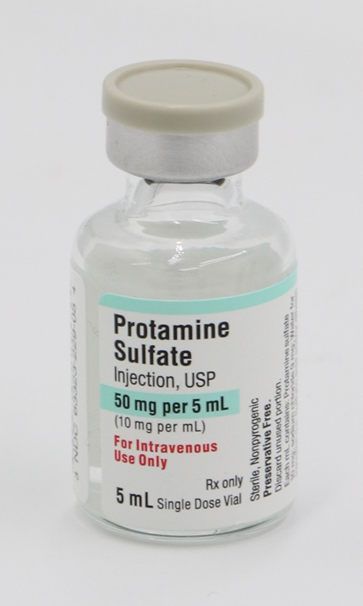
Choice C reason: Protamine is the antidote for heparin, not vitamin K or glucagon. Protamine neutralizes the effects of heparin by binding to it and forming a stable complex.
Choice D reason: Iron is not an antidote for any anticoagulant. Iron is a mineral that is essential for the production of hemoglobin and red blood cells.
Correct Answer is A
Explanation
Choice A reason: Using an electric razor while on warfarin is the correct instruction. Warfarin is an anticoagulant that inhibits the formation of blood clots and prolongs the bleeding time. Using an electric razor can reduce the risk of cuts and bleeding while shaving. The client should avoid using sharp objects or instruments that can cause injury or trauma.
Choice B reason: Doubling the dose of warfarin if a dose is missed is not the correct instruction. This is a dangerous and potentially fatal advice, as it can cause overdose and severe bleeding. The client should take the missed dose as soon as possible, unless it is close to the next scheduled dose, in which case the client should skip the missed dose and resume the regular dosing schedule. The client should never take extra doses or change the dose without consulting the provider.
Choice C reason: Mild nosebleeds being common during initial treatment is not the correct instruction. This is a false and misleading statement, as nosebleeds are not a normal or expected side effect of warfarin therapy. Nosebleeds can indicate bleeding problems or complications, such as thrombocytopenia, which is a low platelet count. The client should report any nosebleeds or other signs of bleeding, such as bruising, petechiae, hematuria, or melena, to the provider immediately.
Choice D reason: Increasing fiber intake to reduce the adverse effect of constipation is not the correct instruction. This is an irrelevant and unnecessary recommendation, as constipation is not a common or serious adverse effect of warfarin therapy. Constipation can be caused by many factors, such as diet, hydration, activity, or medication. The client should maintain a balanced and consistent diet, drink plenty of fluids, and exercise regularly to prevent constipation. The client should also avoid foods that are high in vitamin K, such as green leafy vegetables, as they can interfere with the effect of warfarin.
Whether you are a student looking to ace your exams or a practicing nurse seeking to enhance your expertise , our nursing education contents will empower you with the confidence and competence to make a difference in the lives of patients and become a respected leader in the healthcare field.
Visit Naxlex, invest in your future and unlock endless possibilities with our unparalleled nursing education contents today
Report Wrong Answer on the Current Question
Do you disagree with the answer? If yes, what is your expected answer? Explain.
Kindly be descriptive with the issue you are facing.
