A nurse is caring for a client who asks for information regarding organ donation. Which of the following responses should the nurse make?
Your name cannot be removed once you are listed on the organ donor list
You must be at least 21 years of age to become an organ donor
I cannot be a witness for your consent to donate
Your desire to be an organ donor must be documented in writing
The Correct Answer is D
the correct answer is d. Your desire to be an organ donor must be documented in writing. This is because organ donation is a legal and medical process that requires your consent and documentation1. Some of the other options are incorrect or misleading. Here are some explanations:
- a. Your name can be removed once you are listed on the organ donor list2. You can change your mind at any time and revoke your consent to donate
- b. You do not have to be at least 21 years of age to become an organ donor2. Many states allow people younger than 18 to register as organ donors, but they need parental or guardian consent if they die before their 18th birthday
- c. You can have a witness for your consent to donate, but it is not required1. Some states may require a witness signature on your donor card or registration form, but others do not
Nursing Test Bank
Naxlex Comprehensive Predictor Exams
Related Questions
Correct Answer is A
Explanation
The correct answer is choice A, administer a fluid bolus.
Choice A rationale:
Administering a fluid bolus is appropriate when a client’s urine output is low, which in this case is less than the minimum expected output of 30 mL/hr. The dark yellow color of the urine also suggests dehydration or concentrated urine, which can be addressed with increased fluid intake.
Choice B rationale:
Initiating continuous bladder irrigation is typically done to clear the urinary tract of blood clots or debris following urologic surgery, not for low urine output or dark urine. Therefore, this intervention is not indicated based on the given scenario.
Choice C rationale:
Obtaining a urine specimen for culture and sensitivity is an action taken when there is a suspicion of a urinary tract infection. The scenario does not provide evidence of infection, such as fever or cloudy urine with a strong odor, so this would not be the first intervention to anticipate.
Choice D rationale:
Clamping the catheter tubing is done in preparation for catheter removal or to assess if the client can void without the catheter. It is not an appropriate intervention for low urine output or dark urine and could potentially cause bladder distention or discomfort.
Correct Answer is C
Explanation
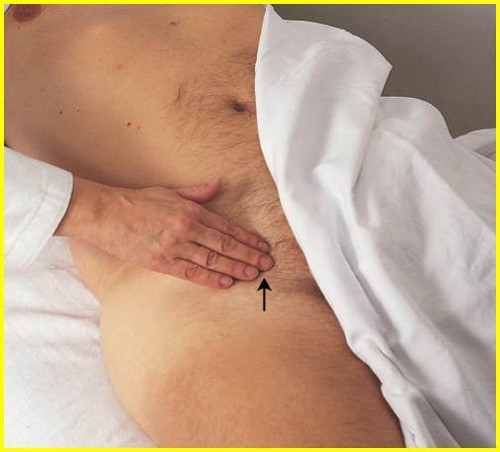
This is because coarctation of the aorta is a congenital condition where the aorta is narrow, usually in the area where the ductus arteriosus inserts. This causes a decrease in blood flow to the lower body, resulting in weak or absent pulses in the femoral arteries.
The other choices are incorrect for the following reasons:
- Choice A, frequent nosebleeds, is not a typical sign of coarctation of the aorta.
Nosebleeds can be caused by many factors, such as dry air, allergies, trauma, or bleeding disorders.
- Choice B, upper extremity hypotension, is also not a common finding in coarctation of the aorta. In fact, patients with this condition may have high blood pressure in the upper extremities due to the increased resistance of the narrowed aorta.
- Choice D, increased intracranial pressure, is not directly related to coarctation of the aorta.
Increased intracranial pressure can be caused by various conditions that affect the brain, such as head injury, stroke, infection, or tumor.
Normal ranges for blood pressure and pulse vary depending on age, sex, and health status.
However, some general guidelines are:
- Blood pressure: less than 120/80 mmHg for adults; less than 95/65 mmHg for infants.
- Pulse: 60 to 100 beats per minute for adults; 100 to 160 beats per minute for infants.
Whether you are a student looking to ace your exams or a practicing nurse seeking to enhance your expertise , our nursing education contents will empower you with the confidence and competence to make a difference in the lives of patients and become a respected leader in the healthcare field.
Visit Naxlex, invest in your future and unlock endless possibilities with our unparalleled nursing education contents today
Report Wrong Answer on the Current Question
Do you disagree with the answer? If yes, what is your expected answer? Explain.
Kindly be descriptive with the issue you are facing.
