A female client is taking alendronate, a bisphosphonate, for postmenopausal osteoporosis. The client tells the nurse that she is experiencing jaw pain. How should the nurse respond?
Determine how the client is administering the medication.
Advise the client to gargle with warm salt water twice daily.
Report the client's jaw pain to the healthcare provider.
Confirm that this is a common symptom of osteoporosis.
The Correct Answer is C
Jaw pain in a client taking alendronate, a bisphosphonate, for postmenopausal osteoporosis may be a sign of a rare but serious side effect called osteonecrosis of the jaw (ONJ). Therefore, the nurse should respond by: Report the client's jaw pain to the healthcare provider.
Jaw pain can be an indication of ONJ, a condition characterized by the death of jawbone tissue. It is important to notify the healthcare provider so that further evaluation and appropriate management can be initiated. The healthcare provider will determine the best course of action, which may include referral to a specialist for further assessment and treatment.
Determining how the client is administering the medication is not the immediate concern in this situation. While it is important to ensure that the client is following proper administration instructions for alendronate, addressing the jaw pain takes precedence.
Advising the client to gargle with warm salt water twice daily may not be sufficient or appropriate for managing jaw pain related to alendronate use. The client needs a comprehensive assessment by the healthcare provider to determine the cause of the jaw pain and provide appropriate interventions.
Confirming that jaw pain is a common symptom of osteoporosis is not accurate. While osteoporosis can lead to bone pain, jaw pain specifically associated with bisphosphonate use is more likely to be related to ONJ and requires further evaluation and management
Nursing Test Bank
Naxlex Comprehensive Predictor Exams
Related Questions
Correct Answer is ["A","D"]
Explanation
Choice A rationale: Hypoxic-ischemic injury from submersion can lead to delayed cerebral edema. Monitoring is critical as the brain's inflammatory response to the initial insult often peaks several hours after the event.
Choice B rationale: Asphyxia is the initial event that occurred in the pool. By the time the child is admitted to the pediatric floor, the asphyxiation event has passed; the nurse now monitors for its aftereffects.
Choice C rationale: Near-drowning victims are more likely to experience hypotension due to myocardial depression or shifting fluid balances. Hypertension is not a typical expected complication in the immediate post-submersion recovery period.
Choice D rationale: Aspiration of water interferes with surfactant production and damages alveolar membranes, leading to pulmonary edema or ARDS. Respiratory status can deteriorate rapidly 6 to 8 hours after the initial insult.
Choice E rationale: The child was in cool water with an outdoor temperature of 64°F, making hypothermia the primary concern. Hyperthermia is not expected unless a secondary infection or a thermregulation failure occurs much later.
Choice F rationale: The head CT scan was negative for bleeding. Without a significant traumatic impact or pre-existing condition, a subdural hemorrhage is not a standard complication resulting from a submersion injury.
Correct Answer is B
Explanation
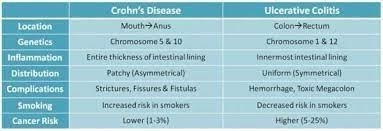
A) Incorrect- Anal abscesses and fistulas are more commonly associated with Crohn's disease than with ulcerative colitis. Crohn's disease can involve the entire thickness of the bowel wall and create tunnels or connections (fistulas) between different parts of the gastrointestinal tract.
B) Correct- Rectal bleeding is a common symptom of ulcerative colitis, as the inflamed tissue can bleed easily.
C) Incorrect- Constipation is not a common characteristic of Crohn's disease. In fact, both ulcerative colitis and Crohn's disease can lead to a range of bowel habits, including diarrhea and constipation, depending on the extent and location of inflammation.
D) Incorrect- Both ulcerative colitis and Crohn's disease are inflammatory bowel diseases (IBD) that involve chronic inflammation of the gastrointestinal tract. Ulcerative colitis primarily affects the colon and rectum, causing continuous areas of inflammation and ulceration. Crohn's disease can affect any part of the gastrointestinal tract, from the mouth to the anus. It often involves patches of inflammation with healthy tissue in between, and it can affect different layers of the bowel wall.
Whether you are a student looking to ace your exams or a practicing nurse seeking to enhance your expertise , our nursing education contents will empower you with the confidence and competence to make a difference in the lives of patients and become a respected leader in the healthcare field.
Visit Naxlex, invest in your future and unlock endless possibilities with our unparalleled nursing education contents today
Report Wrong Answer on the Current Question
Do you disagree with the answer? If yes, what is your expected answer? Explain.
Kindly be descriptive with the issue you are facing.
